Chapter 5: Local Wound Care & Documentation
Authors:
- Joshua Moralejo, RN, BScN, MScCH: WPC, IIWCC (CAN)
- Patricia Coutts, RN, IIWCC (CAN)
- Laurie Goodman, RN, MHScN, IIWCC (CAN)
- Reneeka Jaimangal, MD, MScCH, IIWCC (CAN)
- R. Gary Sibbald, BSc. Md. M.Ed., D.SC (Hon), FRCPC (Med)(Derm), FAAD, MAPWCA, JM
Learning Objectives
- Describe local wound care in supporting the wound environment
- Identify important wound parameters for documentation
This chapter will discuss the following statements from the Wound Bed Prep 2021:
- Statement 4: Local Wound Care – Monitor Wound History and Clinical Examination
- Statement 7: Moisture Management
Local Wound Care
Case Study
A 59-year-old female with history of swelling of feet and ankles at the end of the day. Unremarkable medical history
Developed a left medical malleolus wound from shaking snow off her boot and subsequently hitting her leg on a metal portion of the car. The wound is described as painful at times (up to 5/10 on the numerical 11 point scale), and with increased drainage an occasional odour.
Vascular studies indicated mild incompetence of the left greater saphenous vein, and the ankle-branchial pressure index (ABPI) are 1.12 on the left and 1.00 on the right.
Her partner is very involved in her care assisting with dressing changes including applying compression bandages. Her greatest wish is to be able to walk her dog again without fear of falling.
Question – Describe local wound care consideration for this case.
Local wound care is a practice that involves a series of procedures including cleansing, protection, dressing selection and monitoring (See Local Wound Care Figure 1). Local wound care depends on your patient, a detailed wound assessment, and what is available within the environment and the system. Wound care should also be driven by the wound’s ability to heal. For healable wounds, local wound care interventions can range anywhere along the spectrum from maintaining a moist environment to sharp debridement (Sibbald et al., 2021). On the other hand, treatment of maintenance and non-healable wounds is focused on selective debridement, managing infection, and keeping the wound dry (Sibbald et al., 2021).
Figure 1 – Local Wound Care © Joshua Moralejo & Patricia Coutts
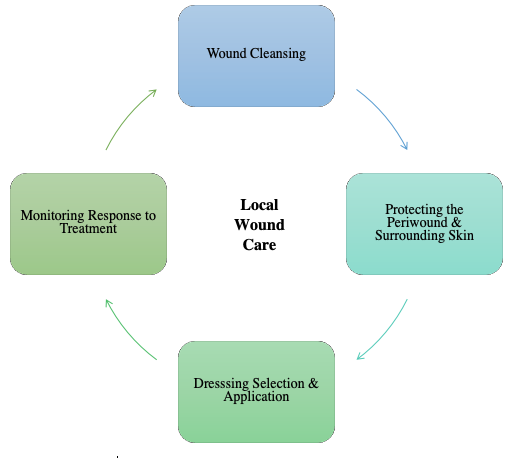
Wound Cleansing
Cleansing wounds are kept simple with gentle techniques using normal saline or potable tap water. Upon dressing removal and disposal, wound odour may be present, and this should disappear after appropriate cleansing. If the wound odour persists after cleansing, the cause should be explored for possible infection. When antiseptics are considered to manage bacteria or infection, then the use of low-toxicity cleansers are encouraged (Sibbald et al., 2015). Antiseptics should only be used when their benefit (antimicrobial action) outweigh the risk (potential cytotoxicity).
Protecting the Periwound and Surrounding Skin
Wound care not only involves cleansing the wound bed, but also the periwound (4cm beyond the wound borders) and surrounding skin. Build-up of debris, dry or dead skin, previous dressing residue or dried, crusted blood along the edges of the wound require gentle cleansing to prevent bacterial growth. After cleansing, the intact skin surrounding the wound should be protected. Skin protectants such as creams or liquid film barriers can be used to prevent potential breakdown such as exposure to wound exudate resulting in maceration (Sibbald et al., 2012).
Dressing Selection and Application
Dressings do not heal wounds; however, they do promote an optimal environment that supports wound healing. It is important to recognize that the wound is on a patient, the patient is in an environment and the environment is within a system. Therefore, a holistic approach in the wound plan of care is essential in optimizing dressing selection.
Dressings are meant for various purposes and are selected based on their function (what they do) and form (how they are designed). Some are made to protect the wound from the external environment, while others are used to promote debridement (e.g. autolytic), manage local infection or inflammation, and reduce or maintain moisture (Sibbald et al., 2021). Wound healing classification will direct dressing selection choices to optimize the desired moisture levels for the wound. Multipurpose dressings also exist e.g. moisture balance, autolytic debridement and antibacterial or a silver alginate.
The traditional categories of dressings include films, hydrogels, hydrocolloids, acrylics, calcium alginates, gelling fibers, foams and super absorbents. Dressings designed to manage exudate have the capacity to absorb scant to very large volumes of exudate. The appropriate size of the dressing should be selected when trying to manage the exudate. These dressings used to manage exudate are further expanded in Wound Bed Preparation 2015 (Sibbald et al 2015). Dressings used to manage local infection have an antimicrobial agent (such as iodine, silver, polyhexamethylenebiguanide [PHMB], chlorhexidine etc.) added to these traditional dressing categories.
There are other tools available to help with the selection of the appropriate local wound care products (See Wounds Canada’s Wound Dressing Selection Guide and Product Picker).
Monitoring and Evaluation
Local wound care interventions should be re-evaluated periodically to ensure that the appropriate wound cleanser and dressings are used to optimize the wound environment. Patient factors such as patient preference, pain, previous products used and response to treatment should also be included in the care planning.

