Considerations and Complications of Offloading
The presence of ischemia and/or infection affects the choice of offloading. Offloading must not impede circulation or exacerbate infection. TCCs can be used in the case of mild ischemia or treated mild infection, but not when both are present (Bus et al., 2020). Knee-high removable cast walkers can be used with caution in the presence of both mild ischemia and mild infection (Bus et al., 2020). However, a referral to a specialty wound clinic may be warranted to assess for the safest choice of offloading in these more complex cases.
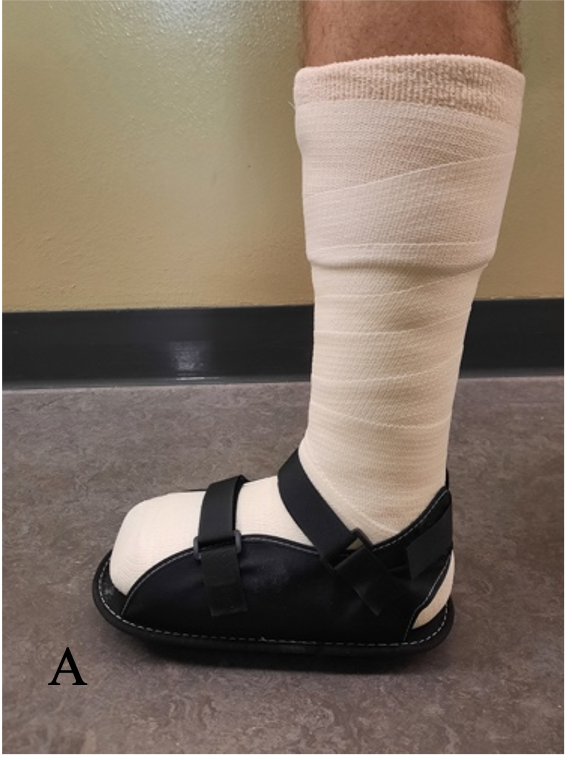
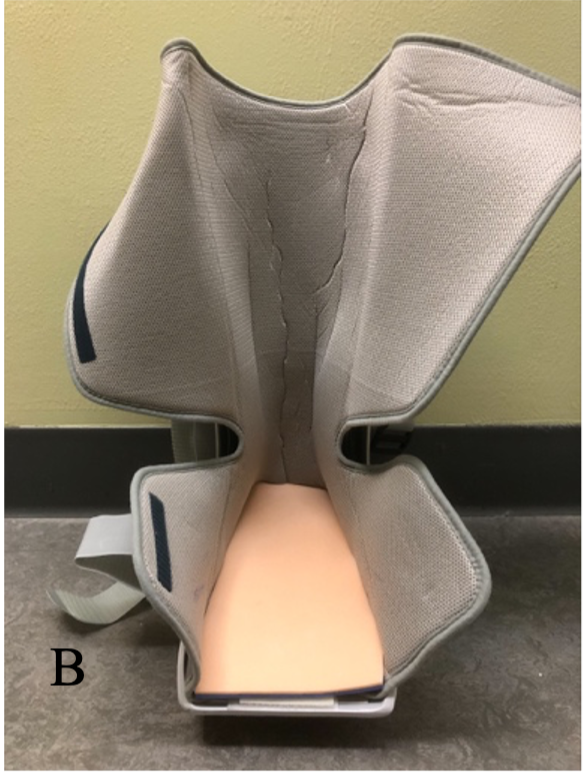
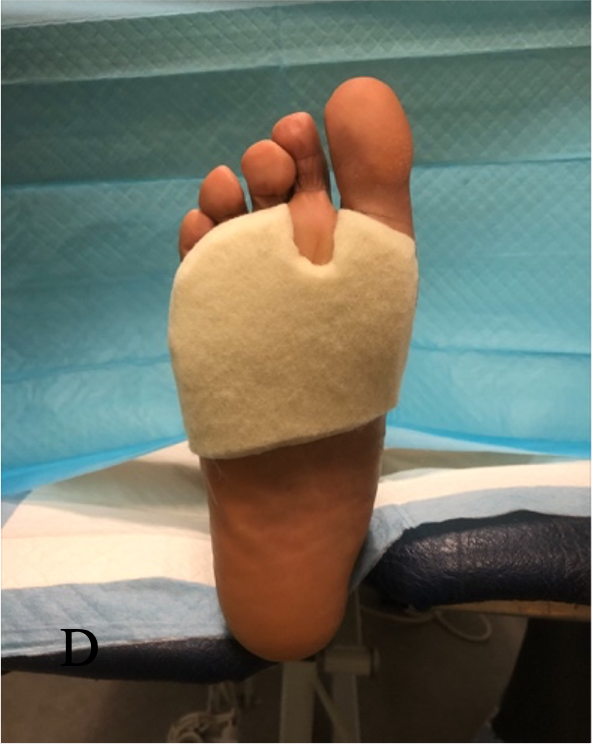
Figure 1 Sample Offloading Devices for DFU
| A
|
B
|
| C
|
D
|
Note: Panel A: TCC with a cast shoe Panel B: Removable cast walker with a plastazote and poron foot-device interface exposed Panel C: Surgical shoe. Panel D: Semi-compressed felt plantar metatarsal pad with “U” cut to offload the right 2nd metatarsal phalangeal joint.
Photos courtesy of Tobi Mark, Eliot To, Nouhad Hamam and Alex Krutow
Patient Education
Patients require instruction on how to don and doff offloading devices. Assess each patient’s gait wearing the device to ensure they are stable and any risk of falls has been mitigated with the use of mobility aids (e.g. canes, walkers and crutches). A medical referral may be necessary to assess for the use of mobility aids and to ensure the home environment is safe for use of the offloading device. A shoe-levelling device can be worn on the contralateral limb to address any leg length discrepancies that may occur due to the offloading worn on the affected foot (Bus et al., 2020; Lazzarini & Jarl, 2021).
Patients must wear their offloading during every step taken, both inside and outside their home, to be effective. Activity modification to decrease the amount of walking and exercise is often necessary. Excessive weight-bearing may cause skin irritation or exacerbate wounds. Clear verbal and written instructions should be given on what to do in case of any adverse events due to the use of an offloading device. Patient education is a process and should be addressed at every clinical visit.
Cost Considerations
Offloading devices have an associated global cost. In Ontario, offloading devices alone are estimated to cost an average of $1425 per patient (Diabetes Canada, n.d.). It is important to be aware of any available local funding strategies, governmental or non-governmental, to subsidize the cost of offloading. Third party insurance may supplement the cost of devices.
Surgical Offloading
Surgery can be used to address underlying structural abnormalities, especially if conservative measures fail (Botros et al., 2019; Bus et al., 2020). Surgical procedures include the digital flexor tenotomy, Achilles’ tendon lengthening, metatarsal head resection and joint arthroplasty (Bus et al., 2020). A referral to a surgeon with a specialty in foot surgery may be required. Surgical options may be maintained with conservative offloading.
Lifelong Offloading
Offloading is a lifelong process. It is important to discuss this concept with patients often so that reasonable expectations are formed incorporating patient-centered concerns. Facilitate discussion to help patients understand how standing on their DFU prolongs healing. Following wound closure, tensile strength of the epithelialized skin of healed wounds is only 80% of that of unwounded skin (Levenson et al., 1965). Healed areas are at risk of future breakdown and new areas of risk may develop over time. Custom inserts, orthotics and orthopedic shoes are often necessary to redistribute pressures across the plantar foot and provide stability. At times, specialized braces may be required. The Charcot Restraint Orthotic Walker (CROW) is designed to offload the Charcot foot. Building a culture of the acceptance of lifelong offloading is critical to treatment success.