Gowns
In healthcare, there are two types of medical gowns: isolation gowns and surgical gowns. Gowns may also be called procedural gowns, non-surgical gowns, or operating-room gowns. Surgical gowns are worn by healthcare providers while performing care in a sterile area. Gowns used for additional precautions are usually called isolation gowns. Isolation gowns are protective garments worn to protect clothing from the splashing or spraying of body fluids and to reduce the transmission of microorganisms (Public Health Ontario, 2020b).
Isolation gowns can be disposable or reusable. The gowns should have long sleeves with a snug fit at the wrist, cover both the front and the back of the body from the neck to the thighs, and overlap at the back (PHO, 2020b). Gowns should fasten at the neck and waist using ties, snaps, or Velcro. A variety of gown sizes should be made available to ensure appropriate coverage for healthcare providers (PIDAC, 2012).
Disposable gowns are made from materials that make them resistant to fluids. Reusable gowns are made of tightly woven cotton or polyester and are chemically finished to improve their ability to be fluid resistant (PHO, 2020b).
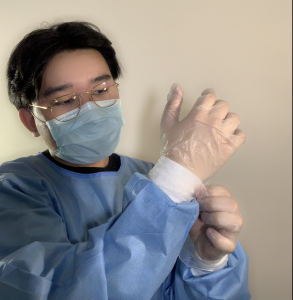
If gloves are being worn with a gown, the gloves should fit over the cuffs of the gown. Gowns are considered task-specific and should be changed if heavily soiled or damaged and should not be reused later. Special care should be taken when removing the gown to prevent contamination of clothing and skin (PIDAC, 2012). The front of the gown is always considered to be contaminated, as are ties at the front. Ties that are at the side and the back are considered to be uncontaminated (Kozier et al, 2018).
Isolation gowns are considered task-specific and are worn only when providing client care. Isolation gowns should be put on immediately prior to the task to be completed with the client and removed immediately after care has been provided.
After use, gowns should be discarded into an appropriate receptacle for disposal, or laundering if the gown is reusable.
Clinical Tip
Some clinical settings might have reusable gowns that are heavy. Wearing full PPE will increase your body temperature, so it’s important to stay hydrated throughout your shift.
Important Considerations when Wearing Gowns
Points of Consideration: Choice of Gown to Use
The choice of gown to use for client care in the clinical setting depends on the following:
- Potential contact with infectious materials.
- Potential that blood and body fluids will penetrate the gown.
Clinical Tips
Practice putting on gowns.
- Practice tying a gown behind your head. Getting your gown on and off quickly in your placement makes a difference. You will not always have that extra minute to untie a knot.
- Tie a lace onto the belt loop of your pants and practice tying it similar to tying the back of the gown. Ensure that your gown is secure! You don’t want your gown falling off while providing client care.
Review Putting it All Together for steps on putting on and taking off a gown.
Attribution
This page was remixed with our own original content and adapted from: Clinical Procedures for Safer Patient Care — Thompson Rivers University Edition by Renée Anderson, Glynda Rees Doyle, and Jodie Anita McCutcheon is used under a CC BY 4.0 Licence. This book is an adaptation of Clinical Procedures of Safer Patient Care by Glynda Rees Doyle and Jodie Anita McCutcheon, which is under a CC BY 4.0 Licence. A full list of changes and additions made by Renée Anderson can be found in the About the Book section.

