Chain of Transmission
The chain of transmission, also referred to as the chain of infection, describes the infection process. There are six links in the chain:
- Infectious Agent
- Reservoirs
- Portal of Exit
- Modes of Transmission
- Portals of Entry
- Susceptible Host
(PIDAC, 2012)
You need to understand how an infectious agent travels throughout the cycle to determine how to break the chain and prevent the transmission of the infectious disease. If a part of the chain of transmission is broken, the infection will not occur. Routine practices and additional precautions are used to break or minimize the chain of transmission.
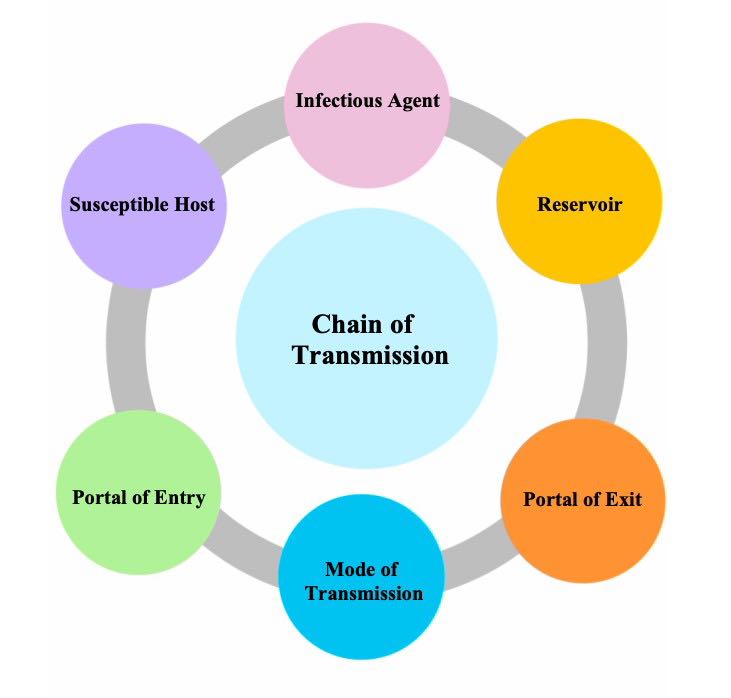
Click on the dropdown button under each chain of transmission link to learn more about that link in the chain and how to break the chain to stop or reduce the transmission of the infection.
To stop the transmission of an infectious agent, at least one link must be broken. To help determine how to break the chain of transmission, perform a risk assessment with every client, in every situation, and in all healthcare settings. When consistently following infection prevention and control measures, you can eliminate the infectious agent transmission.
Points of Consideration: Healthcare Providers and Infectious Agents
Healthcare providers are vulnerable to infectious agents. According to Public Health Ontario (February 21, 2020), 16.6% of healthcare workers have tested positive for COVID-19 in Ontario (https://www.publichealthontario.ca/-/media/documents/ncov/what-we-know-risks-feb-21-2020.pdf?la=en). The majority of the COVID-19 cases were associated with long-term care healthcare settings.
As a healthcare provider, you need to understand your risk of exposure to healthcare-associated infections. One strategy to decrease your risk is staying up to date with your immunizations. Are you up to date with your vaccinations? Are you a vulnerable person?
Another strategy to decrease your risk of HAI is to wear the appropriate PPE. Do you have access to the appropriate PPE required for care? When caring for clients, are you wearing the appropriate PPE? The majority of infections among healthcare providers occur due to improper removal of PPE.
There should be sufficient and accessible PPE in your workplace. If you are unable to access the appropriate PPE, inform your placement preceptor or instructor, the healthcare setting supervisor or manager, and occupational health for further assistance on the specific procedures to obtain the required PPE.
It is important to reflect on your infection prevention and control practices, be aware of the policies and procedures at your healthcare facility, and maintain competency in your infection prevention and control knowledge and skills.
Fun Fact
Mary Mallon, better known as Typhoid Mary, is a famous historical example of an asymptomatic carrier. Mallon was an Irish immigrant worker who cooked for households in and around New York City between 1900 and 1915. In each household, the residents developed typhoid fever (caused by Salmonella typhi) a few weeks after Mallon started working.
In 1906, one family hired George Soper, an expert in typhoid fever epidemics, to determine the cause of the illnesses in their household. Eventually, Soper tracked Mallon down. He discovered that Mallon was a carrier for typhoid but was immune to it herself. Although active carriers had been recognized before, this was the first time that an asymptomatic carrier of infection had been identified.
Microbiology by Nina Parker, Mark Schneegurt, Anh-Hue Thi Tu, Philip Lister, Brian M. Forster is licensed under a CC BY 4.0 Licence.
Test your Knowledge
Case 1
Case 2
Case 3
Putting it All Together
Note: To enlarge the print, you can expand the activity by clicking the arrows in the right upper corner of the text box.
Attribution
This page was remixed with our own original content and adapted from:
Clinical Procedures for Safer Patient Care — Thompson Rivers University Edition by Renée Anderson, Glynda Rees Doyle, and Jodie Anita McCutcheon is used under a CC BY 4.0 Licence. This book is an adaptation of Clinical Procedures of Safer Patient Care by Glynda Rees Doyle and Jodie Anita McCutcheon, which is under a CC BY 4.0 Licence. A full list of changes and additions made by Renée Anderson can be found in the About the Book section.
Microbiology by Nina Parker, Mark Schneegurt, Anh-Hue Thi Tu, Philip Lister, Brian M. Forster is licensed under a CC BY 4.0 Licence.

