COVID-19
COVID-19, also known as SARS-CoV-2, is a highly contagious virus and a serious health threat to individuals. Healthcare providers must be vigilant in infection prevention and control practices to decrease the risk of transmission of COVID-19 and increase safety during client care.
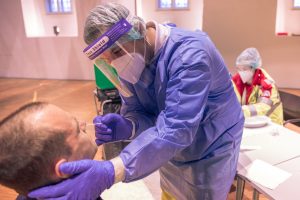
COVID-19 spreads through respiratory droplets and aerosols when an infected person coughs, sneezes, talks, or laughs, and during various medical procedures. The mode of transmission can be contact (direct or indirect), droplet, or airborne. Infectiousness with each mode is still unclear and is continuously being tested by scientists through research. The virus droplets can be large, which land shortly after exiting the respiratory system; for example, when talking, coughing, or sneezing. Or the virus can be smaller, which can linger and travel in the air; for example during aerosol medical procedures. COVID-19 is a new virus and scientists are continuously learning about the microorganism. It is important to continuously educate yourself, as well as clients, about the changing protocols and requirements needed to maintain safety and decrease the risk of transmission.
Watch the following video, Virtual PPE Orientation, to learn about COVID-19 new precautions and information since the beginning of the pandemic. Remember, information is continuously changing and being updated so you must maintain competency in your knowledge.
The risk of contracting COVID-19 varies according to where you live, the client’s presenting symptoms, PPE resources available, health literacy, and human behaviours following infection prevention and control practices. As healthcare providers, knowing the mode of transmission will assist when performing a point-of-care risk assessment.
COVID-19 symptoms vary between people and may take up to 14 days to appear after exposure. People with COVID-19 can be asymptomatic or symptomatic.
COVID-19 Symptoms
Common COVID-19 symptoms can include:
- Temperature equal to or over 37.8°C.
- New or worsening cough.
- Shortness of breath or difficulty breathing.
- Sore throat, runny or congested nose.
- Difficulty swallowing.
- Changes in or loss of smell or taste.
- Gastrointestinal symptoms, including abdominal pain, diarrhea, nausea, vomiting.
(Government of Canada, 2020a; Ontario Ministry of Health, 2020)
Atypical COVID-19 symptoms can include (particularly in infants, children, older persons, and people living with a developmental disability):
- Chills.
- Fatigue or weakness.
- Muscle or body aches.
- Pink eye.
- Headache.
- Feeling very unwell.
- Children tend to feel sluggish, and have abdominal symptoms, lack of appetite and skin changes or rashes.
(Government of Canada, 2020a; Ontario Ministry of Health, 2020)

The older adult population, people living with a developmental disability, pregnant individuals, people with chronic illnesses, people who are immunocompromised, and people living with obesity are at greater risk of serious illness related to COVID-19.
To decrease your risk of contracting or transmitting COVID-19 in the healthcare setting it is essential to maintain competency in the ever-changing information, and to follow required routine practices and additional precautions related to the care that will be provided. (Government of Canada, 2020a; Ontario Ministry of Health, 2020).
Decrease Your Risk of Contracting or Transmitting COVID-19:
- Wear a mask when in public or when in close contact with others.
- Keep 2 meters apart for other individuals outside of your household.
- Wash your hands often with soap and water for a minimum of 20 seconds.
- Avoid touching your face with unwashed hands.
- Avoid closed and crowded places.
- Avoid areas with poor ventilation (re-circulated air).
- Avoid close contact with others. For example, when talking.
- Weather permitting, keep windows open or open periodically to decrease concentration of aerosols inside.

Routine Practices and Additional Precautions
Since COVID-19, the new protocol for routine practices includes a combination of additional precautions: droplet precautions (mask and eye protection) and contact precautions (mask and gloves), because clients that are asymptomatic and pre-symptomatic can transmit infection. When performing an aerosolized procedure (e.g., intubation, high flow nasal oxygen, suctioning a tracheostomy) on COVID-19 clients, airborne precautions such as a, N95 respirator should be used, and a negative pressure room is recommended (PIDAC, 2012, Public Health Ontario, 2021).
Protocols regarding PPE have changed since the COVID-19 pandemic. Public Health Ontario (2021) provides updated guidelines to inform healthcare providers of the minimum expectations regarding PPE. The guidelines address PPE for inpatient facilities, ambulatory and outpatient facilities, and other settings which includes long-term care (Public Health Ontario, 2012). Healthcare providers need to refer to and follow the PPE protocols specific to their healthcare setting. Infection prevention and control protocols are specific to the type of care you provide to a client diagnosed with COVID-19 and according to your healthcare setting. Protocols can vary between sites, units within each site, and the care being provided to the client. COVID-19 protocols are continuously changing according to new discoveries related to COVID-19 and according to PPE availability. It is important to stay up to date on current findings to ensure the safety of yourself and others.
For COVID-19 units, visual cues and a “buddy system” may be used.
- Visual aids help healthcare providers to remember the required steps, how to prevent self-contamination, and decrease the risk of transmission.
- The buddy system can help reduce the risk of contamination when removing PPE. Each healthcare provider watches their buddy as they remove their PPE. The healthcare providers are responsible to ensure the PPE is removed safely during the procedure, stop the other healthcare provider before a potential mistake occurs in the removal technique, and to redirect their buddy’s technique before continuing in the removal of PPE.
Remember it is not about shame or blame; instead it is about safety. Removing PPE is when the highest risk for transmission occurs.
Watch the following video Keeping Yourself Safe During the COVID-19 Pandemic Making the Best use of PPE to learn more about PPE and the steps involved when performing the ‘buddy system’.
Accommodation
Clients diagnosed with COVID-19 should be in a private room or cohort room with another client diagnosed with COVID-19 (Public Health Ontario, 2021). Cohorting healthcare providers should be dedicated and assigned to suspected or confirmed COVID-19 clients only to avoid transmission of the infection to non-suspected or COVID-19 negative clients (Public Health Ontario, 2021). It is recommended to use dedicated break times and areas for COVID healthcare providers within the healthcare setting.
Points of Consideration: COVID-19 Variants
COVID-19 is caused by the SARS-CoV-2 virus. COVID-19 was classified as a pandemic in March 2020. Since the beginning of the COVID-19 pandemic, various variants of the virus have emerged and evolved as the virus is continuously changing.
COVID-19 variants of concern that have emerged in Canada and are on the rise include B.1.1.7 which was first identified in United Kingdom, B.1.351 which was first identified in South Africa, and P.1 which was first identified in Brazil (Government of Canada, 2021, Public Health Ontario, 2021).
Scientists are continuously seeking out and assessing new variants to determine how the virus is changing, how the variant is transmitted, the variant’s effect on humans, severity of the virus, and the vaccines’ effectiveness on the new variants. It is important for you to stay up to date and informed about the continuously changing and new information about COVID-19. As new findings emerge, infection prevention and control practices may change or adapt to address the new findings of the COVID-19 and the variant viruses.
Healthcare providers need to continually promote and educate the public about the importance of hand hygiene, maintaining physical distancing (e.g., 2 meters) with people outside of their household, avoiding crowded spaces and close contact, wearing a mask that covers the nose and goes under the chin, and cleaning their hands often.
Visitors
Currently, visitors are not allowed to physically visit someone diagnosed with COVID-19 when in the hospital. Instead, clients are encouraged to call or video call family and friends, if possible, to connect with them. The healthcare setting infection prevention and control practices related to COVID-19 protocols must be followed.
Client Transportation
The client’s health status, use of medical equipment (e.g., aerosol) and where the client is being transported to and from, will determine which additional precautions to follow. One or a combination of the three additional precautions (contact, droplet and airborne) may be required (PIDAC, 2012).
Cleaning the Environment
COVID-19 can survive on surfaces from hours to days (depending on the surface and environment) if not cleaned properly (Government of Canada, 2020c; Public Health Ontario, 2021). High-touch surface areas should be cleaned and disinfected according to your healthcare facilities environmental service protocol (e.g., at least twice per day and when visibly soiled). The COVID-19 virus can travel via aerosol; therefore, cleaning and disinfecting equipment that uses aerosol and spray bottles should not be used to prevent the transmission of COVID-19 (Public Health Ontario, 2021).
Cohort environmental service staff should be assigned to COVID-19 clients or units if possible. Your healthcare facility should identify a plan for healthcare providers to follow. Where you work and the status of the client will determine how frequently cleaning should take place, the disinfectant contact time, and what cleaning and disinfectant materials should be used. Cleaning and disinfectant materials should be healthcare-grade with a drug identification number (DIN). To learn more about environmental cleaning for COVID-19 review Public Health Ontario (2021) resource COVID-19 Infection Prevention and Control (IPAC) Environmental Services for Health Care Settings https://www.publichealthontario.ca/-/media/event-presentations/pho-webinar-infection-prevention-control-environmental-services.pdf?la=en
Note: Current guidelines are continuously changing as scientists learn more about COVID-19.
Psychosocial Factors
The impact of COVID-19 has been stressful for clients, their care partners, and family. People in the community are also feeling helpless, lonely, and depressed from physical distancing. These responses are normal in a crisis. Healthcare providers can support clients by talking about their fears, clarifying any myths, and educating clients about the most current data on COVID-19.
Healthcare providers are also feeling stressed, uncertain, worried for their own safety, and are experiencing fatigue (Lapum et al., 2020). Further interventions are needed to support healthcare providers’ emotional well-being during this pandemic and continued support will be needed afterwards to address post-pandemic impacts. Remember to check in with your colleagues, as well as yourself, to assess your emotional well-being because it is essential to maintaining your mental health.
Tips for Taking Care of Yourself Include:
- Acknowledge that you are stressed and remember everyone feels stress at times.
- Reach out to family and friends by calling, video chats, or through social platforms to keep connected. It is important to engage with others.

- Practice mindfulness through deep breathing exercises, meditation, and stretching.
- Stay healthy by eating nutritious meals, daily exercising, and getting rest and sleep.
- Keep up to date on new information and follow COVID-19 infection prevention and control protocols.
- Be kind and patient because everyone handles crises differently.
- Be supportive of your family, friends, and community and accept support when you need it.
Test your Knowledge
Attribution
This page was remixed with our own original content and adapted from:
University of Toronto Video:
Video is CC BY NC https://youtu.be/diLN21IGimo. To cite: Caparica Santos, F.N., Matlow, A., and Glover Takahashi, S. Virtual PPE Orientation, June 2020, PGME, University of Toronto. Toronto, Canada. https://pg.postmd.utoronto.ca/the-latest-on-covid-19/
University of Toronto Video:
Keeping Yourself Safe During the Covid-19 Pandemic Making the Best use of PPE. https://youtu.be/PsFGhvlhbXs. For more information visit: https://pg.postmd.utoronto.ca/the-latest-on-covid-19/, cbme.facdev@utoronto.ca Licence: Creative Commons Attribution licence (reuse allowed).

