Common Routes of Transmission
| Site | Associated Risk | Clinical Implications |
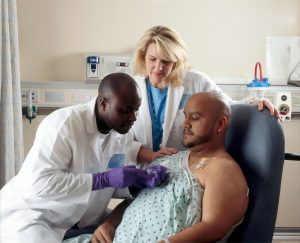
Central Line-Associated Bloodstream Infections (CLABSI) |
Central line is a catheter placed in a large vein to allow: 1) delivery of IV fluids or nutrition 2) blood to be drawn. A central line is larger than an IV line; it typically stays in place longer and can deliver a greater volume of fluids. Because this line is an access portal between a client’s bloodstream and their exterior body, there are associated risks of infection. Central line-associated bloodstream infections (CLABSI) refer to infections of the central line placement that develop within 48 hour and confirmed by the laboratory (Haddadin et al., 2020).
|
Central lines require sterile dressing changes. Dressings over the central line should be clear to observe for signs of infection. The dressing site should have minimal exposure to air. Central lines should be removed as soon as possible and only inserted if necessary. Central lines should be placed above the waist to reduce the risk of contamination. |
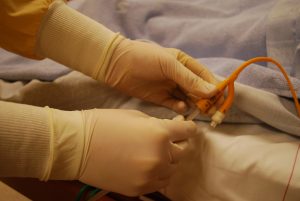
Catheter-Associated Urinary Tract Infections (CAUTI) |
Urinary catheters are hollow, flexible tubes inserted through the urethra into the bladder. These catheters allow drainage of the bladder. They are typically made of rubber, plastic (PVC), or silicone. There are three main types of catheters: indwelling catheters, external catheters and short-term (intermittent) catheters. Because these catheters offer a portal into the bladder with entry near the perineum, there are associated risks of infection (World Health Organization, 2018). The majority of HAIs are associated with urinary catheters. Prolonged use of catheters is associated with increased risk of infection; therefore catheters should only be used when indicated and should be removed once they are no longer needed (World Health Organization, 2018). |
Urinary catheter insertion requires aseptic technique procedure. Don sterile gloves when inserting catheter. Use bladder scan before inserting intermittent catheter to ensure catheterisation is indicated. Daily monitoring of indwelling catheters to ensure it remains in situ is needed. Monitor urine for cloudy, foul smell, or unexplained blood.
|
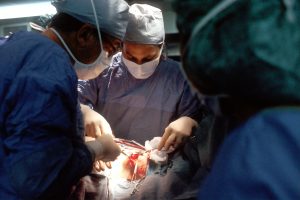
Surgical Site Infection (SSI) |
Surgical site infections occur when harmful bacteria enter the body through the surgical incision. They typically develop shortly after an operation (within 30 days). Some surgeries require clients to take antibiotics pre-operatively to prevent infections. Older client, clients with poor circulation; with weakened immune systems; who smoke, are malnourished, or overweight; or clients with an open incision are at increased risk for surgical site infections. Clients with elevated blood sugar are also at risk for delayed wound healing (Sikora & Zahra, 2020).
|
Perioperatively and post-operatively, healthcare providers should ensure clients have normal body temperature (apply warm-air blanket if necessary). Reduced body temperature deprives the wound of oxygen, rendering it at greater risk for infection. Preoperatively, if hair removal is required, healthcare providers should clip (not shave) any hair that needs to be removed. Small nicks in the skin can make the skin vulnerable to infections. See institutional protocols regarding hair removal and cleansing surgical site prior to surgery. Unless otherwise indicated, wounds should be closed (with stitches) and covered with a sterile dressing for 1-2 days after surgery. If the wound is open, it should be packed with sterile gauze and covered with a sterile dressing. |
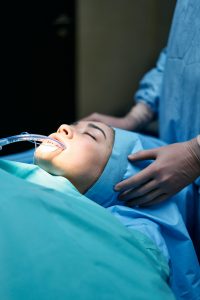
Ventilator-Associated Pneumonia (VAP) |
A ventilator is a machine that mechanically blows air into the lungs in order to maintain proper oxygen levels. A tube can be inserted through the mouth or nose (intubation), or through an opening in the trachea (tracheostomy). Ventilators can be adjusted to meet the needs of clients. Ventilator-associated pneumonia occurs more than 48 hours after the client has been intubated and received mechanical ventilation (Centers for Disease Control and Prevention, 2010).
|
Aggressive surveillance is recommended when clients are on ventilators (e.g., continuous monitoring of signs of infections, vital signs, chest assessment).
|