11.3 – The Organization of the Immune System
The immune system is a collection of barriers, cells, and soluble proteins that interact and communicate with each other in extraordinarily complex ways. The modern model of immune function is organized into a three phases immune response (based on the timing of their effects). Ideally, this response will rid the body of a pathogen entirely (see Figure 11.10).
Think of a primary infection as a race between the pathogen and the immune system:
- The pathogen bypasses barrier defenses and starts to multiply in the host’s body.
- During the first 4 to 5 days, the innate immune response will partially control, but not stop the pathogen growth.
- The slower but more specific and effective adaptive immune response gears up and becomes progressively stronger; it will begin to clear the pathogen from the body. This clearance is referred to as seroconversion. It should be noted that seroconversion does not necessarily mean a patient is getting well.
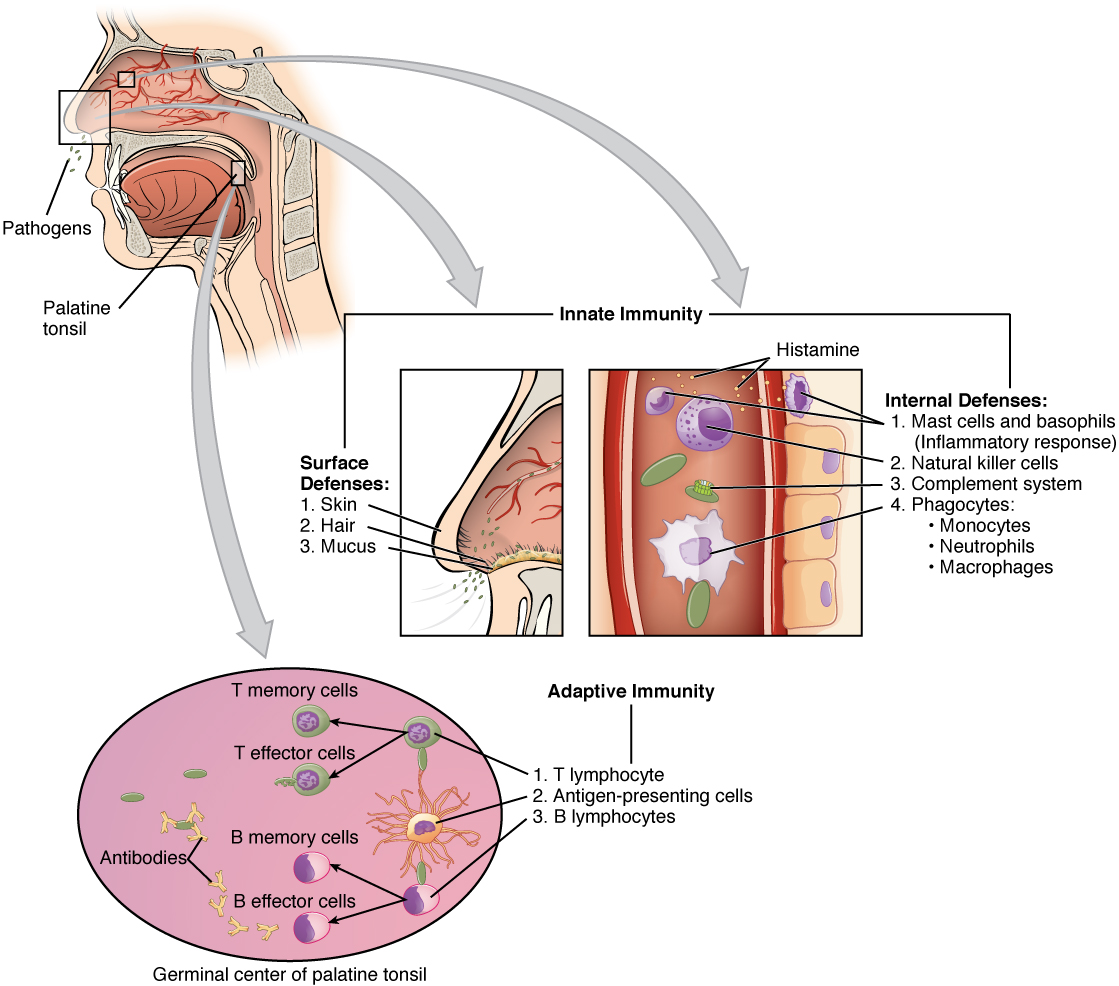
Phase 1: Barrier Defenses
Barrier defenses are part of the body’s most basic innate defense mechanisms. They are not a response to infections, but rather are continuously working to protect against pathogens by preventing them from entering the body, destroying them after they enter, or flushing them out before they can establish themselves.
Barrier defenses examples:
- Skin:
- Keratinized cells of the surface are too dry for bacteria to grow are continuously sloughed off, along with pathogens that are on their surfaces.
- Skin (sweat glands, sebaceous glands):
- Lower pH than pathogens prefer, may contain substances that are toxic to pathogens; washing action.
- Oral cavity (salivary glands):
- Lysozyme is an enxyme that destroys bacteria.
- Stomach:
- Low pH, which is fatal to many pathogens.
- Mucosal:
- Traps both microbes and debris, and facilitates their removal.
- Normal flora (nonpathogenic bacteria):
- Prevents pathogens from growing on mucosal surfaces.
Phase 2: Innate Immune Response
Innate immune responses are critical to the early control of infections. Whereas barrier defenses are the body’s first line of physical defense against pathogens, innate immune responses are the first line of physiological defense. Innate responses occur rapidly, but with less specificity and effectiveness than the adaptive immune response. Within the first few days of an infection, a series of antibacterial proteins are induced, each with activities against certain bacteria. Additionally, interferons are induced that protect cells from viruses in their vicinity. Finally, the innate immune response does not stop when the adaptive immune response is developed. In fact, both can cooperate and one can influence the other in their responses against pathogens.
Innate immune responses (and early induced responses) are in many cases ineffective at completely controlling pathogen growth, but they slow pathogen growth and allow time for the adaptive immune response to strengthen and either control or eliminate the pathogen. The innate immune system also sends signals to the cells of the adaptive immune system, guiding them in how to attack the pathogen.
Watch Immune System, Part 1: Crash Course Anatomy & Physiology #45 (9 min) on YouTube
Media 11.2: Crash Course. (2015, December 08). Immune system, part 1: Crash Course anatomy & physiology #45 [Video]. YouTube. https://youtu.be/GIJK3dwCWCw
Concept Check 1
Do you know the difference between these terms?
Cells of the Innate Immune Response
Phagocytes: Macrophages and Neutrophils
A phagocyte is a cell that is able to surround and engulf a particle or cell, a process called phagocytosis. The phagocytes of the immune system engulf other particles or cells, either to clean an area of debris, old cells, or to kill pathogenic organisms such as bacteria. Macrophages, neutrophils, and dendritic cells are the major phagocytes of the immune system and are the body’s fast acting, front line immunological defense against organisms that have breached barrier defenses and have entered the body.
Macrophages not only participate in innate immune responses but have also evolved to cooperate with lymphocytes as part of the adaptive immune response. Macrophages exist in many tissues of the body, either freely roaming through connective tissues or fixed to reticular fibers within specific tissues such as lymph nodes. When pathogens breach the body’s barrier defenses, macrophages are the first line of defense.
A neutrophil is a phagocytic cell that is attracted via chemotaxis from the bloodstream to infected tissues. contains cytoplasmic granules, which in turn contain a variety of vasoactive mediators such as histamine. Whereas macrophages act like sentries, always on guard against infection, neutrophils can be thought of as military reinforcements that are called into a battle to hasten the destruction of the enemy.
A monocyte is a circulating precursor cell that differentiates into either a macrophage or dendritic cell, which can be rapidly attracted to areas of infection by signal molecules of inflammation.
Natural Killer Cells
NK cells are a type of lymphocyte that have the ability to induce apoptosis in cells infected with pathogens such as intracellular bacteria and viruses. If apoptosis is induced before the virus has the ability to synthesize and assemble all its components, no infectious virus will be released from the cell, thus preventing further infection.
Soluble Mediators of the Innate Immune Response
The previous discussions have alluded to chemical signals that can induce cells to change various physiological characteristics, such as the expression of a particular receptor. These soluble factors are secreted during innate or early induced responses, and later during adaptive immune responses.Cytokines and Chemokines
A cytokine is a signaling molecule that allows cells to communicate with each other over short distances. Cytokines are secreted into the intercellular space, and the action of the cytokine induces the receiving cell to change its physiology. A chemokine is a soluble chemical mediator similar to cytokines except that its function is to attract cells (chemotaxis) from longer distances.
Early Induced Proteins
Early induced proteins are those that are not constitutively present in the body, but are made as they are needed early during the innate immune response. Interferons are an example of early induced proteins. Cells infected with viruses secrete interferons that travel to adjacent cells and induce them to make antiviral proteins. Thus, even though the initial cell is sacrificed, the surrounding cells are protected.
Inflammatory Response
The hallmark of the innate immune response is inflammation. Stub a toe, cut a finger, or do any activity that causes tissue damage, and inflammation will result, with its four characteristics: heat, redness, pain, and swelling (“loss of function” is sometimes mentioned as a fifth characteristic). It is important to note that inflammation does not have to be initiated by an infection, but can also be caused by tissue injuries. The release of damaged cellular contents into the site of injury is enough to stimulate the response, even in the absence of breaks in physical barriers that would allow pathogens to enter (by hitting your thumb with a hammer, for example). The inflammatory reaction brings in phagocytic cells to the damaged area to clear cellular debris and encourages the entry of clotting factors to set the stage for wound repair. Inflammation also facilitates the transport of antigen to lymph nodes by dendritic cells for the development of the adaptive immune response.
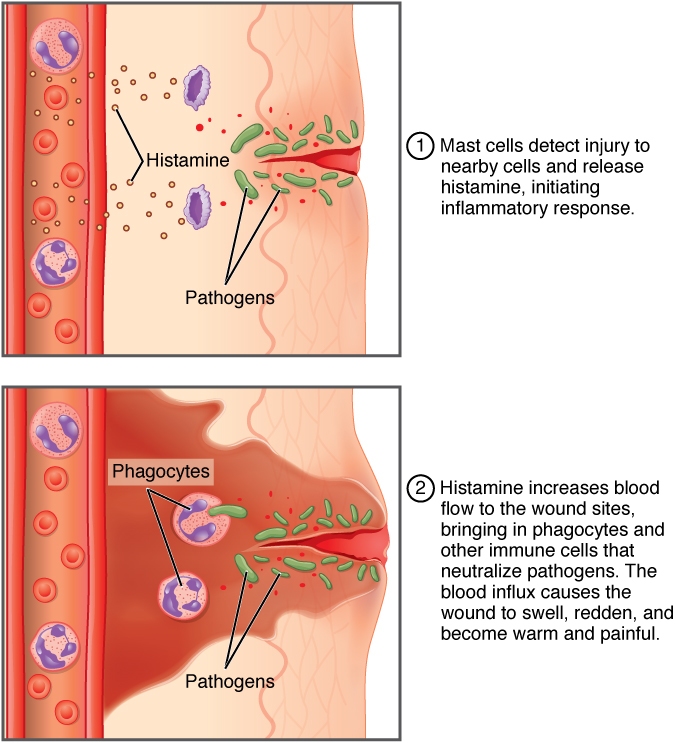
The above image summarizes the following events in the inflammatory response:
- The released contents of injured cells stimulate the release of substances from mast cells including histamine, leukotrienes, and prostaglandins.
- Histamine increases blood flow to the area by vasodilation, resulting in heat and redness. Histamine also increases the permeability of local capillaries, causing plasma to leak out and form interstitial fluid, resulting in swelling.
- Leukotrienes attract neutrophils from the blood by chemotaxis.
- When local infections are severe, neutrophils are attracted to the sites of infections in large numbers, and as they phagocytose the pathogens and subsequently die, their accumulated cellular remains are visible as pus at the infection site.
- Prostaglandins cause vasodilation by relaxing vascular smooth muscle and are a major cause of the pain associated with inflammation. Nonsteroidal anti-inflammatory drugs such as aspirin and ibuprofen relieve pain by inhibiting prostaglandin production.
Concept Check 2
- Do you remember the suffix used to describe ‘inflammation’?
- Describe what causes the pain associated with inflammation.
Acute inflammation is a short-term innate immune response to an insult to the body. If the cause of the inflammation is not resolved, however, it can lead to chronic inflammation, which is associated with major tissue destruction and fibrosis.
Phase 3: Adaptive Immune Response
Watch Immune System, Part 2: Crash Course Anatomy & Physiology #46 (10 min) on YouTube
Media 11.3: CrashCourse (2015, December 14). Immune system, part 2: Crash Course anatomy & physiology #46 [Video]. YouTube. https://youtu.be/2DFN4IBZ3rI
Benefits of the Adaptive Immune Response
- Specificity
- The ability to specifically recognize and mount a response against almost any pathogen.
- Antigens are recognized by receptors on the surface of B and T lymphocytes.
- Immunological Memory
- The first exposure to a pathogen is called a primary adaptive response.
- Symptoms of a first infection, called primary disease, are always relatively severe because it takes time for an initial adaptive immune response to a pathogen to become effective.
- Upon re-exposure to the same pathogen, a secondary adaptive immune response is generated, which is stronger and faster that the primary response, often eliminating the pathogen before it can cause damage or even symptoms.
- This secondary response is the basis of immunological memory, which gives us immunity.
- Self Recognition
- The ability to distinguish between self-antigens, those that are normally present in the body, and foreign antigens, those that might be on a potential pathogen.
- As T and B cells mature, there are mechanisms in place that prevent them from recognizing self-antigen, preventing a damaging immune response against the body. When these mechanisms fail, their breakdown leads to autoimmune diseases.
Lymphocytes: B Cells, T Cells, Plasma Cells
As stated above, lymphocytes are the primary cells of adaptive immune responses. These cells were introduced in the previous chapter and are summarized in the following table:
| Cell Type |
Description and Details |
|---|---|
| Plasma Cell | B cell (lymphocyte) that has been activated through exposure to an antigen and produces antibodies against that antigen (see the figure below) There are 5 classes of antibodies (IgM, IgG, IgE, IgA, IgD), each functioning in different ways: |
IgM promotes chemotaxis, opsonization, and cell lysis, making it a very effective antibody against bacteria at early stages of a primary antibody response
IgG is the one that crosses the placenta to protect the developing fetus from disease and exits the blood to the interstitial fluid to fight extracellular pathogens
IgA is the only antibody to leave the interior of the body to protect body surfaces. IgA is also of importance to newborns, because this antibody is present in mother’s breast milk (colostrum), which serves to protect the infant
IgE is associated with allergies and anaphylaxis
T Cell
Different T cell types have the ability to either secrete soluble factors that communicate with other cells of the adaptive immune response or destroy cells infected with intracellular pathogen.
- Cytotoxic T Cell (Tc) kill target cells by inducing apoptosis using the same mechanism as NK cells: killing a virally infected cell before the virus can complete its replication cycle results in the production of no infectious particles.
- Helper T Cell (Th) release cytokines, which help to develop and regulate other immune system cells.
- Suppressor T Cell (also called regulatory T cell) control T Cell response, in order to prevent too many T cells from being formed during an immune response.
Memory B Cell cells and T cells formed during primary exposure to a pathogen (see the figure below) remain in the body for a long time after an infection and are able to mount a fast and effective immune response to a pathogen if it is encountered a second time, preventing the pathogen from causing disease.
Active Versus Passive Immunity
Immunity to pathogens, and the ability to control pathogen growth so that damage to the tissues of the body is limited, can be acquired by:
- The active development of an immune response in the infected individual.
or - The passive transfer of immune components from an immune individual to a non-immune one.
The downside to this passive immunity is the lack of the development of immunological memory. Once the antibodies are transferred, they are effective for only a limited time before they degrade.
| Immunity | Natural | Artificial |
|---|---|---|
| Active: resistance to pathogens acquired during an adaptive immune response | Result of memory cells formed during the adaptive immune response to a pathogen | Vaccine response. Through vaccination, one avoids the disease that results from the first exposure to the pathogen, yet reaps the benefits of protection from immunological memory. Vaccination was one of the major medical advances of the twentieth century and led to the eradication of smallpox and the control of many infectious diseases, including polio, measles, and whooping cough |
| Passive: transfer of antibodies from an immune person to a nonimmune person | Trans-placental antibodies from mother to fetus and maternal antibodies in breast milk protect newborn from infections | Immunoglobulin injections taken from animals previously exposed to a specific pathogen; a fast-acting method of temporarily protecting an individual who was possibly exposed to a pathogen |
Evasion of the Immune System by Pathogens
The immune system and pathogens are in a slow, evolutionary race to see who stays on top. Early childhood is a time when the body develops much of its immunological memory that protects it from diseases in adulthood. Pathogens have shown the ability, however, to evade the body’s immune responses, as described below.
- Protective adaptations: It is important to keep in mind that although the immune system has evolved to be able to control many pathogens, pathogens themselves have evolved ways to evade the immune response. An example is in Mycobactrium tuberculosis, which has evolved a complex cell wall that is resistant to the digestive enzymes of the macrophages that ingest them, and thus persists in the host, causing the chronic disease tuberculosis.
- Multiple strains: Bacteria sometimes evade immune responses because they exist in multiple strains, each having different surface antigens and requiring individual adaptive immune responses. One example is a small group of strains of S. aureus, called methicillin-resistant Staphylococcus aureus (MRSA), which has become resistant to multiple antibiotics.
- Antigen mutation: Because viruses’ surface molecules mutate continuously, viruses like influenza change enough each year that the flu vaccine for one year may not protect against the flu common to the next. New vaccine formulations must be derived for each flu season.
- Genetic recombination: An example is the influenza virus, which contains gene segments that can recombine when two different viruses infect the same cell. Recombination between human and pig influenza viruses led to the 2010 H1N1 swine flu outbreak.
- Immunosuppression: Pathogens, especially viruses, can produce immunosuppressive molecules that impair immune function.
Tissue Transplantation
With the use of tissue typing and anti-rejection drugs, transplantation of organs and the control of the anti-transplant immune response have made huge strides in the past 50 years.
Immunosuppressive drugs such as cyclosporine A have made transplants more successful, but tissue matching is still key. Family members, since they share a similar genetic background, are much more likely to share MHC molecules than unrelated individuals do.
One disease of transplantation occurs with bone marrow transplants, which are used to treat various diseases, including SCID and leukemia. Because the bone marrow cells being transplanted contain lymphocytes capable of mounting an immune response, and because the recipient’s immune response has been destroyed before receiving the transplant, the donor cells may attack the recipient tissues, causing graft-versus-host disease. Symptoms of this disease, which usually include a rash and damage to the liver and mucosa, are variable, and attempts have been made to moderate the disease by first removing mature T cells from the donor bone marrow before transplanting it.
Immune Responses Against Cancer
It is clear that with some cancers, like Kaposi’s sarcoma (see Figure 11.14), for example, that a healthy immune system does a good job at controlling them. This disease, which is caused by the human herpes virus, is almost never observed in individuals with strong immune systems. Other examples of cancers caused by viruses include liver cancer caused by the hepatitis B virus and cervical cancer caused by the human papilloma virus. As these last two viruses have vaccines available for them, getting vaccinated can help prevent these two types of cancer by stimulating the immune response.
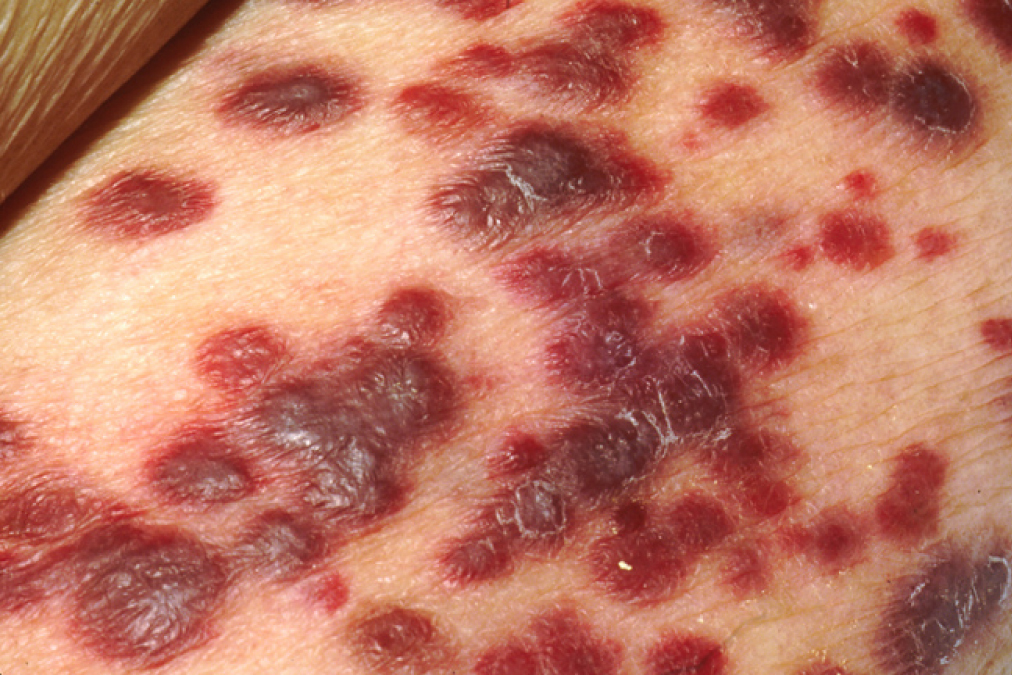
On the other hand, as cancer cells are often able to divide and mutate rapidly, they may escape the immune response, just as certain pathogens, such as HIV, do.
There are three stages in the immune response to many cancers:
- Elimination occurs when the immune response first develops toward tumor-specific antigens specific to the cancer and actively kills most cancer cells.
- Equilibrium is the period that follows, during which the remaining cancer cells are held in check.
- Escape of the immune response, and resulting disease, occurs because many cancers mutate and no longer express any specific antigens for the immune system to respond to.
This fact has led to extensive research in trying to develop ways to enhance the early immune response to completely eliminate the early cancer and thus prevent a later escape. One method that has shown some success is the use of cancer vaccines. These differ from other vaccines in that they are directed against the cells of one’s own body. Treated cancer cells are injected into cancer patients to enhance their anti-cancer immune response and thereby prolong survival. The immune system has the capability to detect these cancer cells and proliferate faster than the cancer cells do, thus overwhelming the cancer in a similar way as they do for viruses. Cancer vaccines are being developed for malignant melanoma and renal (kidney) cell carcinoma.
Immune Responses and Stress
In order to protect the entire body from infection, the immune system is required to interact with other organ systems, sometimes in complex ways. For example, hormones such as cortisol (naturally produced by the adrenal cortex) and prednisone (synthetic) are well known for their abilities to suppress T cell immune mechanisms, hence, their prominent use in medicine as long-term, anti-inflammatory drugs.
One well-established interaction of the immune, nervous, and endocrine systems is the effect of stress on immune health. In the human vertebrate evolutionary past, stress was associated with the fight-or-flight response, largely mediated by the central nervous system and the adrenal medulla. This stress was necessary for survival since fighting or fleeing usually resolved the problem in one way or another. It has been found that short-term stress diverts the body’s resources towards enhancing innate immune responses. This has the ability to act fast and would seem to help the body prepare better for possible infections associated with the trauma that may result from a fight-or-flight exchange.
On the other hand, there are no physical actions to resolve most modern day stresses, including short-term stressors like taking examinations and long-term stressors such as being unemployed or losing a spouse. The effect of stress can be felt by nearly every organ system, and the immune system is no exception (see Table 11.3). Chronic stress, unlike short-term stress, may inhibit immune responses even in otherwise healthy adults. The suppression of both innate and adaptive immune responses is clearly associated with increases in some diseases.
| System | Stress-Related Illness |
|---|---|
| Integumentary system | Acne, skin rashes, irritation |
| Nervous system | Headaches, depression, anxiety, irritability, loss of appetite, lack of motivation, reduced mental performance |
| Muscular and skeletal systems | Muscle and joint pain, neck and shoulder pain |
| Circulatory system | Increased heart rate, hypertension, increased probability of heart attacks |
| Digestive system | Indigestion, heartburn, stomach pain, nausea, diarrhea, constipation, weight gain or loss |
| Immune system | Depressed ability to fight infections |
| Male reproductive system | Lowered sperm production, impotence, reduced sexual desire |
| Female reproductive system | Irregular menstrual cycle, reduced sexual desire |
Immune System Medical Terms
Medical Terms Not Easily Broken into Word Parts
Lymphatic System Medical Terms Not Easily Broken Down (Text Version)
Practice the following lymphatic system words by breaking into word parts and pronouncing.
- allergen
- Substance capable of producing an allergic (hypersensitivity) reaction
- Allergist
- Specialist who studies and treats allergies
- allergy
- inflammatory response due to a hypersensitivity to a substance
- acute inflammation
- Inflammation occurring for a limited time period, rapidly developing
- afferent lymphatic vessels
- vessels that lead into a lymph node
- antibody
- antigen-specific protein secreted by plasma cells, immunoglobulin
- antigen
- molecule recognized by the receptors of b and t lymphocytes
- chronic inflammation
- Inflammation occurring for long periods of time
- chyle
- lipid-rich lymph inside the lymphatic capillaries of the small intestine
- efferent lymphatic vessels
- vessels that lead out of a lymph node
- erythroblastosis fetalis
- Also called HDN (hemolytic disease of newborn) disease of RH-positive newborns in RH-negative mothers with multiple RH-positive children. Resulting from the action of maternal antibodies against fetal blood.
- Graft-versus-host disease (GVHD)
- In bone marrow transplants, occurs when the transplanted cells mount an immune response against the recipient
- immunological memory
- ability of the adaptive immune response to mount a stronger and faster immune response upon re-exposure to a pathogen
- innate immune response
- rapid but relatively non-specific immune response
- lymph
- fluid contained within the lymphatic system
- lymph node
- one of the bean-shaped organs found associated with the lymphatic vessels
- Severe combined immunodeficiency disease (SCID)
- Genetic mutation that affects both t cell and b cell arms of the immune response
- Spleen
- Secondary lymphoid organ that filters pathogens from the blood and remove degenerating or damage blood cells
- Thymus
- Primary lymphoid organ, where t lymphocytes proliferate and mature
- Tonsils
- Lymphoid nodules associated with the nasopharynx
- vaccine
- An agent administered by injection, orally or nasal spray that provides active acquired immunity to a particular infectious disease.
- Apoptosis
- Programmed Cell Death
- Bone Marrow
- tissue found inside bones, the site of all blood cell differentiation and maturation of b lymphocytes
- Immunity
- Post infection, memory cells remain in the body providing an immune response to the same pathogen. This protects us from getting sick by the same pathogen
- Histamine
- Vasoactive mediator in granules of mast cells
Primary cause of allergies and anaphylactic shock
- Vasoactive mediator in granules of mast cells
- Inflammation
- Immune response characterized by heat, redness, pain, and swelling
- Interstitial
- Between cells of the tissues
- Interstitial Space
- Spaces between individual cells in the tissues
- Passive Immunity
- Transfer of immunity (usually by injection of antibodies) to a pathogen by an individual who lacks immunity.
Activity source: Endocrine System Medical Terms by Kimberlee Carter, from Building a Medical Terminology Foundation by Kimberlee Carter and Marie Rutherford, licensed under CC BY- 4.0. / Converted to Text.
Lymphatic and Immune System Abbreviations
Lymphatic System Common Abbreviations
- AIDS (acquired immunodeficiency syndrome)
- CBC and DIff (complete blood count and differential)
- GVHD (Graft-versus-host Disease)
- Hct (hematocrit)
- HDN (hemolytic disease of the newborn)
- Hgb (hemoglobin)
- HIV (human immunodeficiency virus)
- IV (Intravenous)
- SCID (severe combined immunodeficiency)
- SPECT (single-photon emission computed tomography)
- WBC (White Blood Cell)
Activity source: Lymphatic System Common Abbreviations by Kimberlee Carter, from Building a Medical Terminology Foundation by Kimberlee Carter and Marie Rutherford, licensed under CC BY- 4.0. /Text version added.
Image Descriptions
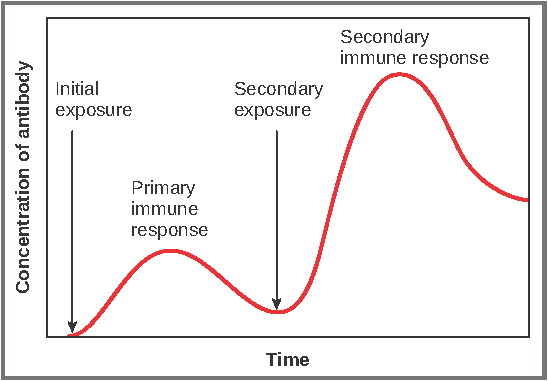
Figure 11.12 image description: This graph shows the antibody concentration as a function of time in primary and secondary response. Initial exposure indicates a low concentration of antibody, which then elevates over time during the primary immune response. It decreases a little during secondary exposure, but then spikes during the secondary immune response. [Return to Figure 11.12].
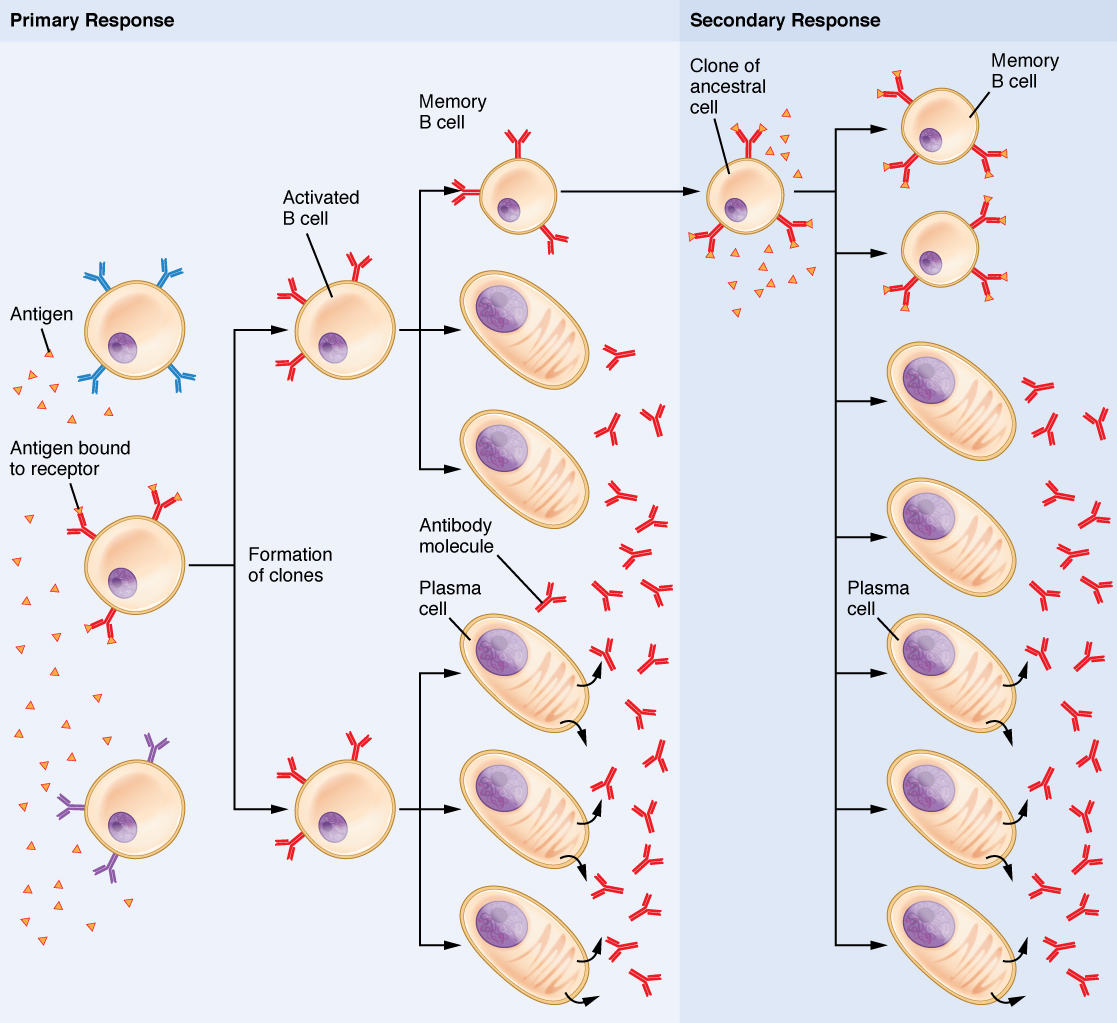
Figure 11.13 image description: This flow chart shows how the clonal selection of B cells takes place. The left panel shows the primary response and the right panel shows the secondary response. During a primary B cell immune response, both antibody-secreting plasma cells and memory B cells are produced. These memory cells lead to the differentiation of more plasma cells and memory B cells during secondary responses. [Return to Figure 11.13].
Attribution
Except where otherwise noted, this chapter is adapted from “Lymphatic and Immune Systems” in Building a Medical Terminology Foundation by Kimberlee Carter and Marie Rutherford, licensed under CC BY 4.0. / A derivative of Betts et al., which can be accessed for free from Anatomy and Physiology (OpenStax). Adaptations: dividing Lymphatic and Immune Systems chapter content into subchapters.
The body's first line of defense against pathogens, a physical barrier to keep pathogens out of the body
Fast-acting non-specific immune mechanisms that are present from birth
Specific immune mechanisms (against a specific pathogen) which take time to develop
Seroconversion is the reciprocal relationship between virus levels in the blood and antibody levels. As the antibody levels rise, the virus levels decline, and this is a sign that the immune response is being at least partially effective. Partially, because in many diseases, seroconversion does not necessarily mean a patient is getting well.(Betts et al., 2013)
Mucous membranes line body cavities that open to the outside world, including the respiratory tract, gastrointestinal tract, urinary tract and reproductive tracts
Early induced proteins made in virally infected cells that cause nearby cells to make antiviral proteins (Betts et al., 2013)
Between cells
Inside the cell membrane or within the cell
Between cells of the tissues, often used interchangeably with 'intercellular'
also phagocytosed, this is the process by which certain cells are able to 'eat' other cells or substances by engulfing them
programmed cell death
The smooth muscle layer in the wall of the blood vessel relaxes, allowing the vessel to widen. This decreases blood pressure in the vessel.
Movement in response to chemicals; a phenomenon in which injured or infected cells and nearby leukocytes emit the equivalent of a chemical “911” call, attracting more leukocytes to the site.
Chronic inflammation is ongoing inflammation that can be caused by foreign bodies, persistent pathogens, and autoimmune diseases such as rheumatoid arthritis (Betts et al., 2013)
A substance that provokes an immune response. This happens because the immune system sees the antigen as foreign, or 'non-self" (does not belong in that body)
After an infection, memory cells remain in the body for a long time and can very quickly mount an immune response against the same pathogen if it tries to re-infect. This protects us from getting diseases from the same pathogen over again.
also called immunoglobulins, proteins produced by B lymphocytes in response to a non-self antigen
An antibody or an antimicrobial protein binds to a pathogen, thereby marking it as a target for phagocytes.
Also called anaphylaxis. An inhaled, ingested or injected (bee sting) allergen causes a significant drop in blood pressure along with contractions of smooth muscles of the airways
chemical that sends a message from one cell to another
A vaccine is a killed or weakened pathogen or its components that, when administered to a healthy individual, leads to the development of immunological memory (a weakened primary immune response) without causing much in the way of symptoms (DeSaix et al., 2013)
Staphylococcus aureus is a bacteria that is commonly found in minor skin infections, as well as in the nose of some healthy people
the combining of gene segments from two different pathogens
The determination of MHC molecules in the tissue to be transplanted to better match the donor to the recipient
Major Histocompatibility Complex molecules, also called Human Leukocyte Antigen (HLA) are protein structures found on the outside of cells that help the immune system recognize non-self antigens
Severe combined immunodeficiency disease. Patients have essentially no adaptive (specific) immune system due to genetic defects which affect B cells and T cells
A cancer involving an abundance of leukocytes. It may involve only one specific type of leukocyte from either the myeloid line (myelocytic leukemia) or the lymphoid line (lymphocytic leukemia). In chronic leukemia, mature leukocytes accumulate and fail to die. In acute leukemia, there is an overproduction of young, immature leukocytes. In both conditions the cells do not function properly (Betts, et al., 2013)
GVHD: in bone marrow transplants; occurs when the transplanted cells (the 'graft') mount an immune response against the recipient's (the 'host') tissue

