8.3 Types of Genetic Tests
How are genetic screening tests different from genetic diagnostic tests?
Screening tests evaluate an individual’s risk of developing a genetic condition, while diagnostic tests identify genetic conditions. All genetic tests have both benefits and limitations.
Genetic screening tests are generally used in people who do not have signs or symptoms of a disorder. These tests estimate whether an individual’s risk of having a certain condition is increased or decreased compared with the risk in other people in a similar population. A positive result means that a person’s risk of developing the condition is higher than average. A negative screening test means that a person’s risk is lower than average. However, having a positive screening result does not mean the individual has the condition. Because screening tests are only estimates, the results, in some cases, indicate an increased risk for a genetic abnormality when the person is unaffected (false positive), or the results indicate a decreased risk for a genetic abnormality when the person is affected (false negative). While genetic screening tests do not provide a conclusive answer, they can help guide the following steps, such as whether additional diagnostic testing is needed.
Genetic diagnostic tests are often used in people who have signs and symptoms. These tests are used to confirm or rule out suspected genetic conditions. Diagnostic tests can also help inform a person’s chance of developing a genetic condition or passing it to their children. Diagnostic testing can be performed before birth or at any time during a person’s life, but it is not available for all genes or all genetic conditions. The results of a diagnostic test can be used to guide a person’s choices about health care and the management of the disorder.
Concept in Action
Watch Genetic Testing’s Impact on Patient Care – Page’s Story (4 mins) on YouTube to learn how genetic testing can impact a patient’s diagnostic odyssey.
Video source: Mayo Clinic. (2017, October 26). Genetic testing’s impact on patient care – Paige’s Story [Video]. YouTube. https://youtu.be/-UHg0oEqdAg
How are genetic tests performed?
Genetic tests are performed on a sample of blood, hair, skin, amniotic fluid (the fluid that surrounds a fetus during pregnancy), or other tissue. For example, a buccal (pronounced buh-kl) smear uses a small brush or cotton swab to collect a sample of cells from the inside surface of the cheek. Depending on the suspected disorder, the sample is sent to a laboratory where technicians look for genetic variants in chromosomes, DNA, or proteins. If requested, the laboratory reports the test results in writing to a person’s doctor, genetic counsellor, or patient. Before a person has a genetic test, it is important to obtain informed consent to be sure they understand the testing procedure, the benefits and limitations of the test, and the possible consequences of the test results. The International Society of Nurses in Genetics (ISONG) has a position statement on informed decision-making related to genetic testing and the nurse’s role [PDF].
Examples of genetic screening tests
Reproductive genetic carrier screening Carrier screening supports informed decision-making for prospective parents by identifying couples at higher risk of having a child affected by a severe genetic condition, whether autosomal or X-linked recessive (Henneman et al., 2016; Plantinga et al., 2016; Yao et al., 2016). The optimal time to discuss carrier screening is during the preconception period, when individuals are planning pregnancy, or at a woman’s first prenatal visit, regardless of gestational age (Edwards et al., 2015; Wilson et al., 2016). Current Canadian and international guidelines recommend offering carrier screening based on an individual’s ethnic background or the presence of specific personal or family history risk factors (Edwards et al., 2015; Henneman et al., 2016; Wilson et al., 2016). Canadian recommendations for Point of Care tools on reproductive genetic screening are available. “Expanded carrier screening refers to reproductive genetic carrier screening beyond one’s ethnicity and family history” (GECKO, n.d.-d).
Noninvasive prenatal testing/screening (NIPT/NIPS): This screening test is performed before birth to help determine the risk that a fetus will be born with certain genetic abnormalities, such as Down syndrome and other chromosomal disorders (MedlinePlus, n.d.-a).
For more information, see GECKO on the run: Non-invasive prenatal testing (NIPT) – a 2-page, evidence-based summary for healthcare providers. Features include current Canadian recommendations, red flags to consider regarding the offer of NIPT, what the results mean, and the benefits and limitations of the test.
Prenatal Screening is available to all pregnant women in Canada. Different methods are used for prenatal screening, depending on the purpose and gestation. Here is a comprehensive guide to understanding prenatal screening [PDF], an excellent patient resource (GECKO, n.d.-c).
With prenatal screening and detailed second-trimester ultrasound, the chance to have a baby with some specific genetic conditions or developmental differences can be more precisely determined. Prenatal screening is about risk assessment [PDF]. (GECKO, n.d.-c).
Newborn screening tests (NBS) are done shortly after birth on a small blood sample (blood spot), taken by pricking the baby’s heel. A nurse places a few drops of blood onto a special filter paper attached to a blood spot card (Perinatal Services BC, 2024). A NBS tests for treatable disorders that manifest their symptoms during childhood and are not otherwise easily identifiable at birth. This allows for early diagnosis and treatment. Unlike other types of genetic testing, a parent will usually only receive the result if it is positive. If the test result is positive, additional testing is needed to determine whether the baby has a genetic disorder. ISONG also has a position statement on newborn screening and the nurses’ role [PDF]. (MedlinePlus, 2023).
In Canada, each province is responsible for how it distributes health care funding and programming. Genetic services, including NBS, differ from province to province. The number of conditions screened for ranges from 14-36 (Groulx-Boivin et al., 2024). This creates a lack of equity in healthcare treatment across the country. Ongoing advocacy exists to establish a national NBS program (Canadian MPS Society, 2022).
Cascade testing tests family members of an individual with a pathogenic/likely pathogenic variants, usually who is affected by the condition. This process identifies other family members at risk of the hereditary condition (NCI, n.d).
Examples of genetic diagnostic tests
Molecular gene tests: These tests determine the order of DNA building blocks (nucleotides) in an individual’s genetic code, a process called DNA sequencing. Molecular tests can also analyze RNA. The purpose of these tests is to identify pathogenic genetic variants. Molecular tests include polymerase chain reaction (PCR), fluorescent in situ hybridization (FISH) and next-generation sequencing (NGS) (MedlinePlus, n.d.-b).
Targeted single variant testing
Single variant tests look for a specific variant in one gene. The selected variant is known to cause a disorder (for example, the particular variant in the HBB gene that causes sickle cell disease). This type of test is often used to test family members of someone known to have a particular variant to determine whether they have a familial condition (MedlinePlus, n.d.-b).
Single gene testing
Single gene tests –Single gene tests look for any genetic changes in one gene. These tests are typically used to confirm (or rule out) a specific diagnosis, mainly when many variants in the gene can cause the suspected condition (CDC, 2024).
Genetic panel testing
Multigene panels – Panel tests look for variants in more than one gene. This type of test is often used to pinpoint a diagnosis when a person has symptoms that may fit a wide array of conditions or when the suspected condition can be caused by variants in many genes. (For example, there are hundreds of genetic causes of epilepsy) MedlinePlus, n.d.-b).
Large-scale genomic testing
Two methods, whole exome sequencing and whole genome sequencing, are increasingly used in healthcare and research to identify genetic variations; both methods rely on new technologies that allow rapid sequencing of large amounts of DNA. These approaches are next-generation sequencing (or next-gen sequencing) (CDC, 2024).
- Whole exome sequencing looks at all the genes in the DNA (whole exome) or those related to medical conditions (clinical exome). (MedlinePlus, n.d.-b; CDC, 2024).
- Whole genome sequencing is the most significant genetic test and looks at all of a person’s DNA, not just the genes. (MedlinePlus, n.d.-b; CDC, 2024).
The original sequencing technology, called Sanger sequencing (named after the scientist who developed it, Frederick Sanger), was a breakthrough that helped scientists determine the human genetic code, but it was time-consuming and expensive. The Sanger method has been automated to make it faster and is still used in laboratories today to sequence short pieces of DNA, but it would take years to sequence a person’s genome. Next-generation sequencing has sped up the process (taking only days to weeks to sequence a human genome) while reducing costs (Medline Plus, n.d.c).
With next-generation sequencing, it is now feasible to sequence large amounts of DNA, for instance, all of an individual’s exons, the DNA that provides instructions for making proteins, which are thought to make up 1 percent of a person’s genome. Together, all the exons in a genome are known as the exome. In whole exome sequencing, variations in the protein-coding region of any gene are identified, rather than in only a select few genes. Because most known variants that cause disease occur in exons, whole exome sequencing is considered an efficient method to identify possible disease-causing variants (Medline Plus, n.d.c).
However, researchers have found that DNA variations outside the exons can affect gene activity and protein production and lead to genetic disorders–variations that whole exome sequencing would miss. Whole genome sequencing determines the order of all the nucleotides in an individual’s DNA and can determine variations in any part of the genome (Medline Plus, n.d.c).
Whole exome sequencing or whole genome sequencing are tests that analyze the bulk of an individual’s DNA to find genetic variations. Whole exome or whole genome sequencing is typically used when a single gene or panel testing has not provided a diagnosis or when the suspected condition or genetic cause is unclear. Whole exome or whole genome sequencing is often more cost- and time-effective than performing multiple single gene or panel tests (MedlinePlus, n.d.-b).
Chromosomal tests: These tests analyze whole chromosomes or long lengths of DNA to identify large-scale changes, such as an extra or missing copy of a chromosome (trisomy or monosomy, respectively) or abnormalities of large segments of chromosomes, that underlie certain genetic conditions(MedlinePlus, n.d.-b).
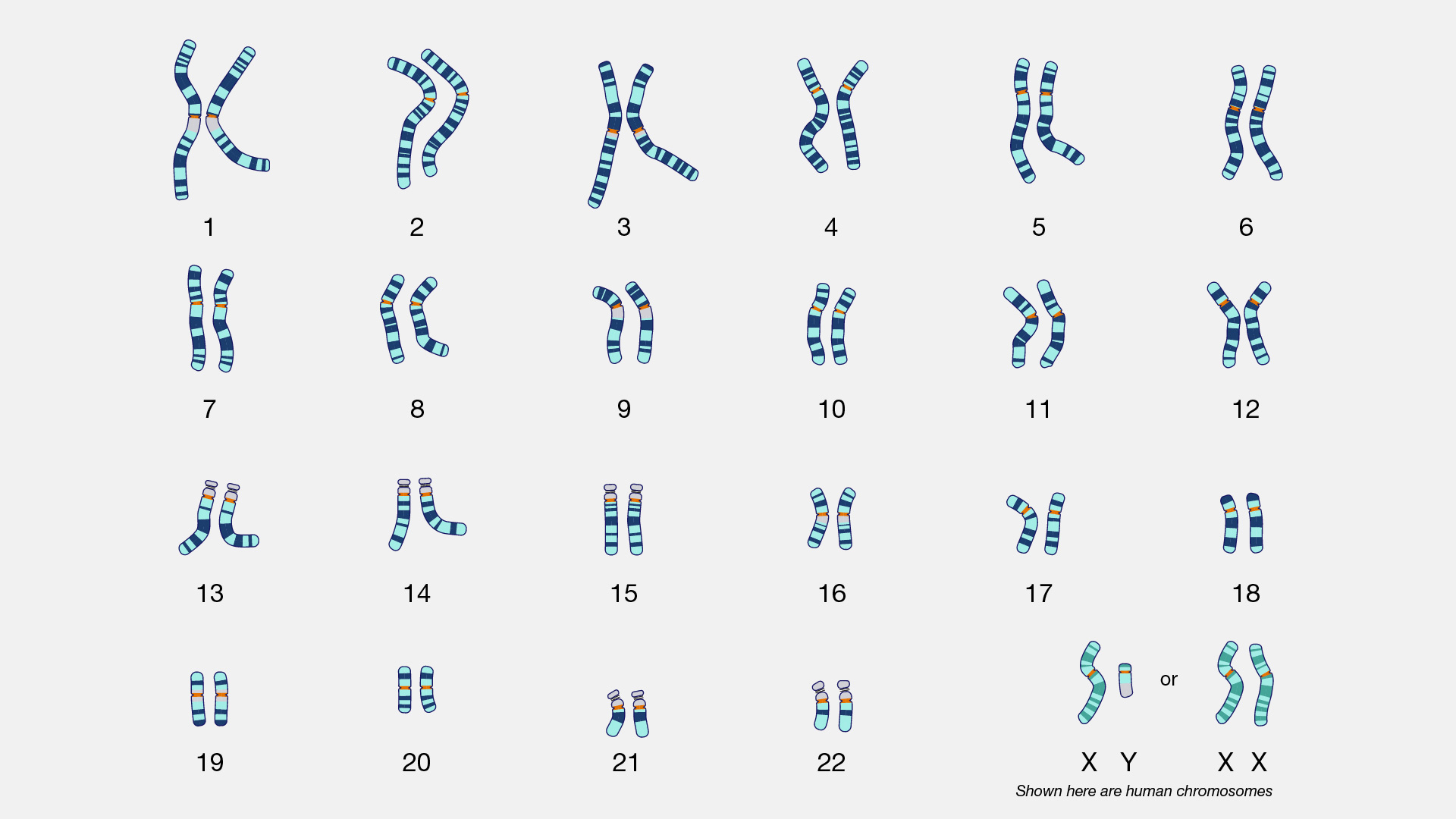
A chromosomal microarray is a newer technology that might be recommended for a child with autism spectrum disorder. A karyotype is a high-level genomic test that analyses the number and structure of an individual’s chromosomes (GECKO, n.d.-a).
More information on chromosomal microarrays vs karyotyping is available here [PDF]. Additionally, see GECKO on the Run: Chromosomal microarray – a 2-page, evidence-based summary for healthcare providers. Features a bottom line, red flags to consider microarray testing and genetic referral, what the results mean, and resources.
Concept in Action
Watch Chromosomal Microarray Testing (4 mins) from Alberta Health Services on YouTube to learn about chromosomal microarray testing.
Video source: MyHealth.Alberta.ca. (2022, March 22). Chromosomal microarray testing [Video]. YouTube. https://www.youtube.com/watch?v=ZrDANI0KSNU
Other tests
A full description of each of these tests is beyond the scope of this course. However, nurses may encounter these in research papers’ methods sections. Therefore, it is beneficial to have a basic overview.
Gene expression tests
Genes are expressed, or turned on, at different levels in different types of cells. Gene expression tests compare these levels between normal and diseased cells because knowing the difference can provide important information for treating the disease. For example, these tests can guide chemotherapy treatment for breast cancer (MedlinePlus, n.d.-b).
Biochemical tests
These tests look at levels or activity of proteins or enzymes produced by genes. Any abnormalities can signify underlying genetic disorders (MedlinePlus, n.d.-b). Metabolomics is a form of biochemical testing where levels of metabolites are measured. Samples such as urine, serum, and plasma can be tested for metabolites. Metabolomics is an emerging area of genetic research. Other forms of biochemical testing include protein assays such as colorimetric assays, immunoassays such as enzyme-linked immuno-absorbent assay (ELISA), mass spectrometry or gel electrophoresis (e.g. Western Blotting).
Epigenetic biomarkers
Other tests used in a clinical context include those looking for epigenetic markers. This is a rapidly evolving area of medical genetics research. Check out Epi-Sign, used to obtain definitive diagnoses when other methods have returned uncertain results. This test examines DNA methylation patterns (biomarkers) associated with specific genetic disorders.
What is circulating tumour DNA, and how is it used to diagnose and manage cancer?
Circulating tumour DNA (ctDNA) is found in the bloodstream and refers to DNA from cancerous cells and tumours. Most DNA is inside a cell’s nucleus. As a tumour grows, cells die and are replaced by new ones. The dead cells get broken down, and their contents, including DNA, are released into the bloodstream. ctDNA are small pieces of DNA, usually comprising fewer than 200 building blocks (nucleotides) in length.
The quantity of ctDNA varies among individuals and depends on the type of tumour, its location, and the cancer stage of cancerous tumours.
Detection of ctDNA can be helpful in the following cases:
- Detecting and diagnosing a tumour. Because tumour DNA has acquired multiple genetic variants, leading to tumour development, ctDNA is not an exact match to the individual’s DNA. Finding DNA with genetic differences aids in tumour detection. Diagnosing the type of tumour using ctDNA can reduce the need to get a tumour tissue sample (tumour biopsy), which can be challenging when a tumour is difficult to access, such as a tumour in the brain or lung.
- Guiding tumour-specific treatment. Analyzing the genome of tumour cells using ctDNA can help doctors determine which treatment will be most effective. However, approval from the U.S. Food and Drug Administration for ctDNA testing to personalize cancer treatment is limited.
- Monitoring treatment. A decrease in the quantity of ctDNA suggests the tumour is shrinking, and treatment is successful.
- Monitoring periods with no symptoms (remission of cancer). A lack of ctDNA in the bloodstream indicates that the cancer has not returned.
Clinical versus direct-to-consumer genetic tests
Clinical genetic tests are different from direct-to-consumer (DTC) genetic tests. A healthcare provider orders clinical genetic tests for a specific medical reason—an individual cannot order this type of testing. In contrast, anyone can buy DTC tests online (CDC, 2024). Other names for direct-to-consumer genetic testing include DTC genetic testing, direct-access genetic testing, at-home genetic testing, and home DNA testing. Ancestry testing (genealogy testing) is also considered a form of direct-to-consumer genetic testing (MedlinePlus, n.d.-d).
Many companies currently offer direct-to-consumer genetic tests for a variety of purposes. The most popular tests use a limited set of genetic variations to make predictions about certain aspects of health, provide information about common traits, and offer clues about a person’s ancestry. The number of companies providing direct-to-consumer genetic testing and the range of health information these tests provide is growing. Because there is currently little regulation of direct-to-consumer genetic testing services, assessing the quality of available services before pursuing any testing (MedlinePlus, n.d.-d).
DTC test results can be used to decide lifestyle choices or identify issues to discuss with a healthcare provider. However, DTC tests cannot determine for sure whether or not the individual will get a disease. Nor should these tests be used alone to make decisions about treatment or medical care or in place of clinical genetic testing. However, patients present to medical professionals with reports generated from DTC testing. Therefore, healthcare providers must be aware that these tests exist and may be sought out by individuals who can pay for them (MedlinePlus, n.d.-d).
For more information, see GECKO on the run: Direct-to-consumer genomic testing – a 3-page, evidence-based summary for healthcare providers. Features include result interpretation, benefits and limitations of testing, and resources (GECKO, n.d.-d). The National Human Genome Research Institute also has an excellent resource on DTC testing for consumers.
ISONG has a position statement on DTC genetic testing [PDF]. It concerns issues of informed consent, misinterpretation of test results, psychosocial concerns, confidentiality, privacy, and integrity of specimens. The Canadian Medical Association also has a position statement on DTC genetic testing [PDF], which considers the role of government and systems infrastructure in regulating DTC testing.
The Office of the Privacy Commissioner of Canada provides good consumer resources on privacy and DTC testing.
Attribution & References
Except where otherwise noted, this section is adapted from
- How are genetic screening tests different from genetic diagnostic tests? In Help Me Understand Genetics by MedlinePlus, Public Domain
- How is genetic testing done? In Help Me Understand Genetics by MedlinePlus, Public Domain
- What is circulating tumour DNA, and how is it used to diagnose and manage cancer? In Help Me Understand Genetics by MedlinePlus, National Library of Medicine, Public Domain with attribution
- Biochemical tests & Epigenetic biomarkers sections written by Andrea Gretchev, CC BY-NC 4.0
References
Canadian MPS Society. (2022). What is newborn screening? https://www.mpssociety.ca/newborn-screening/
CDC. (2024, May 15). Genetic testing. Genomics and Your Health. https://www.cdc.gov/genomics-and-health/about/genetic-testing.html
Edwards, J. G., Feldman, G., Goldberg, J., Gregg, A. R., Norton, M. E., Rose, N. C., Schneider, A., Stoll, K., Wapner, R., & Watson, M. S. (2015). Expanded carrier screening in reproductive medicine-points to consider: a joint statement of the American College of Medical Genetics and Genomics, American College of Obstetricians and Gynecologists, National Society of Genetic Counselors, Perinatal Quality Foundation, and Society for Maternal-Fetal Medicine. Obstetrics and Gynecology, 125(3), 653–662. https://doi.org/10.1097/AOG.0000000000000666
Genetics Education Canada: Knowledge Organization (GECKO). (n.d.-a). GECKO on the run: Chromosomal microarray. https://www.geneticseducation.ca/resources-for-clinicians/genomic-technologies/chromosomal-microarray/gecko-on-the-run-7
Genetics Education Canada: Knowledge Organization (GECKO). (n.d.-b). GECKO on the run: Genomic test results. https://www.geneticseducation.ca/resources-for-clinicians/genomic-technologies/genomic-test-results/gecko-on-the-run
Genetics Education Canada: Knowledge Organization (GECKO). (n.d.-c). Guide to understanding prenatal screening. https://www.geneticseducation.ca/resources-for-the-public/guide-to-understanding-prenatal-screening
Genetics Education Canada: Knowledge Organization (GECKO). (n.d.-d). Point of care tool. https://www.geneticseducation.ca/resources-for-clinicians/genomic-technologies/expanded-carrier-screening/point-of-care-tool-9
Groulx-Boivin, E.,Osman, H., Chakaborty, P., Lintern, S., Oskoui, M., Selby, K., Van Caeseele, P., Wyatt, A., & McMillan, H. J. (2024). Variability in newborn screening across Canada: Spinal muscular atrophy and beyond.” Canadian Journal of Neurological Sciences, 51(2), 203–09. https://doi.org/10.1017/cjn.2023.34.
Henneman, L., Borry, P., Chokoshvili, D., Cornel, M. C., van El, C. G., Forzano, F., Hall, A., Howard, H. C., Janssens, S., Kayserili, H., Lakeman, P., Lucassen, A., Metcalfe, S. A., Vidmar, L., de Wert, G., Dondorp, W. J., & Peterlin, B. (2016). Responsible implementation of expanded carrier screening. European Journal of Human Genetics, 24(6), e1-e12. https://doi.org/10.1038/ejhg.2015.271
MedlinePlus. (n.d.-a). How are genetic screening tests different from genetic diagnostic tests?: MedlinePlus Genetics. https://medlineplus.gov/genetics/understanding/testing/differenttests/
MedlinePlus. (n.d.-b). What are the different types of genetic tests?: MedlinePlus Genetics. https://medlineplus.gov/genetics/understanding/testing/types/
MedlinePlus. (n.d.-c). What are whole exome sequencing and whole genome sequencing?: MedlinePlus Genetics. https://medlineplus.gov/genetics/understanding/testing/sequencing/
MedlinePlus. (n.d.-d). What is direct-to-consumer genetic testing?: MedlinePlus Genetics. https://medlineplus.gov/genetics/understanding/dtcgenetictesting/directtoconsumer/
MedlinePlus. (2023, April 25). Newborn screening tests. MedlinePlus Medical Encyclopedia. https://medlineplus.gov/ency/article/007257.htm
Plantinga, M., Birnie, E., Abbott, K. M., Sinke, R. J., Lucassen, A. M., Schuurmans, J., Kaplan, S., Verkerk, M. A., Ranchor, A. V., & van Langen, I. M. (2016). Population-based preconception carrier screening: how potential users from the general population view a test for 50 serious diseases. European Journal of Human Genetics, 24(10), 1417–1423. https://doi.org/10.1038/ejhg.2016.43
National Cancer Institute (NCI). (n.d.). Cascade screening. In NCI Dictionary of Genetics Terms. https://www.cancer.gov/publications/dictionaries/genetics-dictionary/def/cascade-screening
National Society of Genetic Counselors. (2023, June 15). Secondary and incidental findings in genetic testing [position statement]. https://www.nsgc.org/POLICY/Position-Statements/Position-Statements/Post/secondary-and-incidental-findings-in-genetic-testing-1
Perinatal Services BC. (2024). Newborn blood spot card screening. http://www.perinatalservicesbc.ca/our-services/screening-programs/newborn-screening-bc
Wilson, R. D., De Bie, I., Armour, C. M., Brown, R. N., Campagnolo, C., Carroll, J. C., Okun, N., Nelson, T., Zwingerman, R., Audibert, F., Brock, J. A., Brown, R. N., Campagnolo, C., Carroll, J. C., De Bie, I., Johnson, J. A., Okun, N., Pastruck, M., Vallée-Pouliot, K., Wilson, R. D., … Van Karnebeek, C. (2016). Joint SOGC-CCMG Opinion for Reproductive genetic carrier screening: An update for all Canadian providers of maternity and reproductive healthcare in the era of direct-to-consumer testing. Journal of Obstetrics and Gynaecology Canada, 38(8), 742–762.e3. https://doi.org/10.1016/j.jogc.2016.06.008
Yao, R., & Goetzinger, K. R. (2016). Genetic carrier screening in the twenty-first xentury. Clinics in Laboratory Medicine, 36(2), 277–288. https://doi.org/10.1016/j.cll.2016.01.003

