6.6 Polygenic Risk Scores
Beyond Family History: Sporadic and Non-Heritable Diseases
Not all the characterized human traits and diseases are attributed to mutant alleles at a single gene locus. Many diseases that have a heritable component, have more complex inheritance patterns due to (1) the involvement of multiple genes, and/or (2) environmental factors. On the other hand, some non-genetic diseases may appear to be heritable because they affect multiple members of the same family, but this is due to the family members being exposed to the same toxins or other environmental factors (e.g., in their homes).
Finally, diseases with similar symptoms may have different causes, some of which may be genetic while others are not. One example of this is Amyotrophic lateral sclerosis (ALS); approximately 5–10% of cases are inherited in an AD pattern, while most of the remaining cases appear to be sporadic, in other words, not caused by a variant inherited from a parent. We now know that different genes or proteins are affected in the inherited and sporadic forms of ALS. The physicist Stephen Hawking and baseball player Lou Gehrig both suffered from sporadic ALS.
Watch the video Neuroscience: Amyotrophic Lateral Sclerosis (ALS)video (2 mins), by Neuroscientifically Challenged (2017) on YouTube, which describes how ALS arises in humans.
Video source: Neuroscientifically Challenged. (2017, March 14). 2-ninute neuroscience: Amyotrophic Lateral Sclerosis (ALS) [Video]. YouTube. https://youtu.be/kOnk9Hh20eg
Polygenic Risk
Concept in Action
Watch this What Your Family History Can’t Tell you (7 mins) on YouTube to learn about how genes can interact to create a combined risk for developing disease.
Video source: SciShow. (2019, November 11). What your family history can’t tell you [Video]. YouTube. https://www.youtube.com/watch?v=tkJhdXt2G8k
Calculating polygenic risk scores
Researchers identify genomic variants associated with complex diseases by comparing the genomes of individuals with and without those diseases. The enormous amount of genomic data now available enables researchers to calculate which variants tend to be found more frequently in groups of people with a given disease. There can be hundreds or even thousands of variants per disease. Researchers put this information into a computer and use statistics to estimate how the collection of a person’s variants affect their risk for a certain disease.
This yields polygenic risk scores. A polygenic risk score is one way by which people can learn about their risk of developing a disease, based on the total number of changes related to the disease. All of this can be done without knowing the specific genes involved in the complex disease. While we may someday know all the genes involved, researchers can estimate risk now without this link.
Interpreting polygenic risk scores
A polygenic risk score can only explain the relative risk for a disease. Why relative? The data used for generating a polygenic risk score comes from large scale genomic studies. These studies find genomic variants by comparing groups with a certain disease to a group without the disease.
A polygenic risk score tells you how a person’s risk compares to others with a different genetic constitution. However, polygenic scores do not provide a baseline or timeframe for the progression of a disease. For example, consider two people with high polygenic risk scores for having coronary heart disease. The first person is 22 years old, while the latter is 98. Although they have the same polygenic risk score, they will have different lifetime risks of the disease. Polygenic risk scores only show correlations, not causations.
Absolute risk is different. Absolute risk shows the likelihood of a disease occurring. Women who carry a BRCA1 variant have a 60-80% absolute risk of breast cancer. This would be true even without any comparison to any groups of people.

Who benefits from a polygenic risk score?
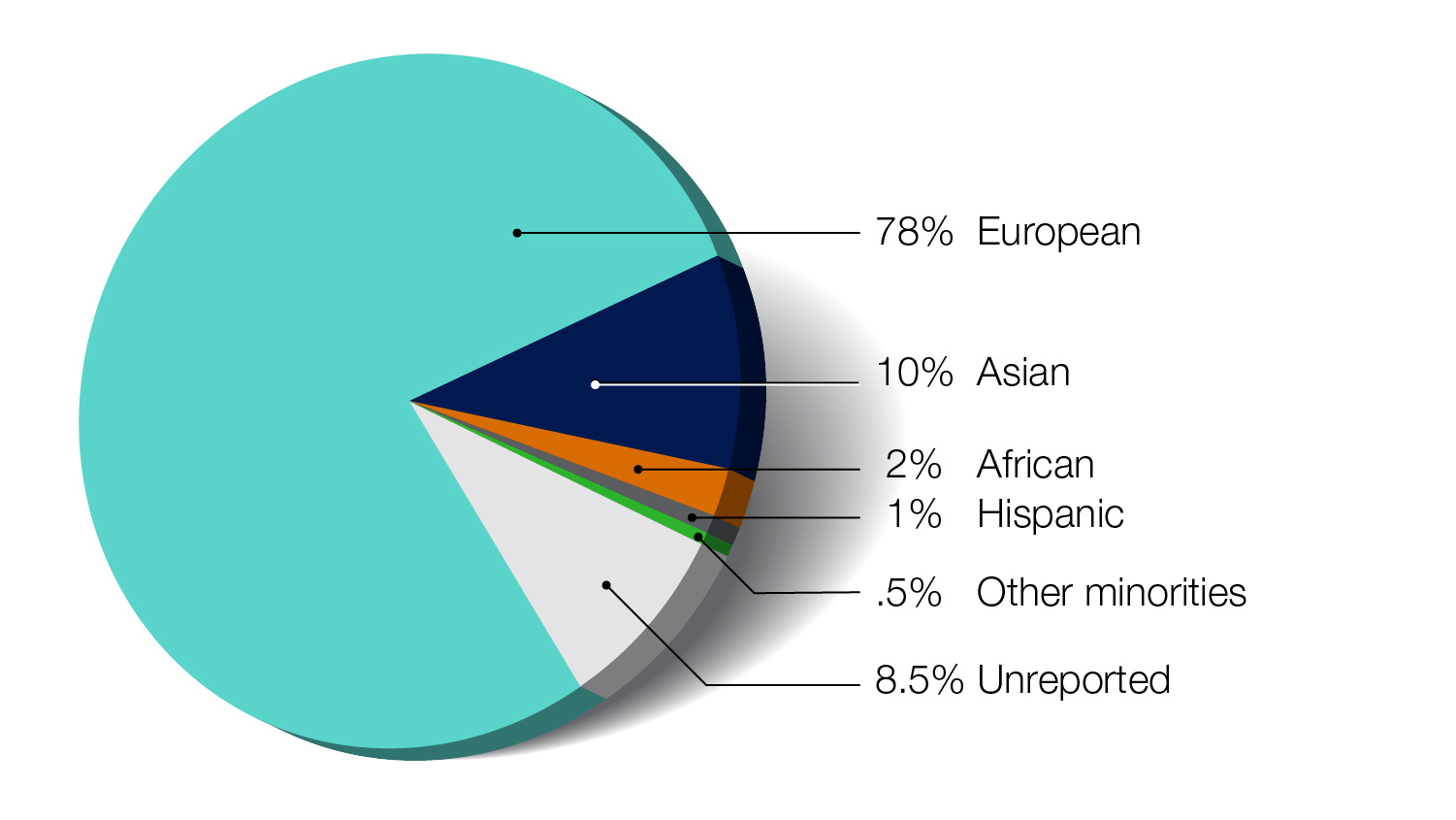
Because the majority of genomic studies to date have examined individuals of European ancestry, there may not be adequate data about genomic variants from other populations for calculating a polygenic risk score in those populations. This historic lack of diversity in genomic studies is also a concern for other genomics-related research areas and contributes to a widespread concern about increasing health disparities beyond polygenic risk scores. At this point in time, the accuracy of polygenic risk scores may only be valid and useful for European ancestry populations. More research is needed to derive the data for making polygenic risk scores useful for other populations.
Looking into the future
Polygenic risk scores are not yet routinely used by health professionals because there are no guidelines for practice and researchers are still improving how these scores are generated. However, private healthcare and direct-to-consumer companies (private commercial companies that individuals can pay for out-of-pocket) have already begun generating polygenic risk scores for their consumers and they may someday serve as an important new tool to guide healthcare decisions.
Polygenic risk scores will always be probabilities, not certainties. Understanding how polygenic risk scores can impact peoples’ lives and health is an active area of research being supported by the National Human Genome Research Institute.
Attribution & References
Except where otherwise noted, this section is adapted from
- 4.4 Sporadic and Non-Heritable Diseases In Introduction to Genetics by Natasha Ramroop Singh, Thompson Rivers University, CC BY-NC-SA 4.0
- Polygenic risk scores courtesy: National Human Genome Research Institute (NHGRI), Public Domain with attribution
References
Mayo Clinic Staff (n.d.). Amyotrophic lateral sclerosis (ALS). MayoClinic.org. https://www.mayoclinic.org/diseases-conditions/amyotrophic-lateral-sclerosis/symptoms-causes/syc-20354022

